This blog post was updated on 3/7/17 to add information.
Being diagnosed with COPD is scary. It leads to endless questions about your future and what it means for you and your family.
It can leave you feeling guilty for possibly causing the onset of the disease from smoking. And it can leave you thinking "Well, now what?"
The truth is, yes COPD is scary and overwhelming, but COPD does not define you and it most certainly is NOT a death sentence.
There are so many different stories from people who are living with moderate to severe COPD that show you can live a high quality life if you take care of yourself and the disease.
For example, Russell Winwood, The COPD Athlete, has one of the most inspiring stories we have come across. Although he is not affiliated with 1st Class Medical in any way, his story is something to marvel at.
Russell has stage 4 COPD and continues to train for triathlons, different Iron Man competitions, and much more! You can read more about Russell and his story here!
Now, this post isn't going to give you the secret on how you can become the next COPD athlete, but it's going to help you understand the different stages of COPD and how you can proactively treat the disease to live a high quality life!
So, let's get to it:
COPD Stage 1 (Mild)

Stage 1 COPD is where you want to catch the disease to be diagnosed. However, due to the lack of symptoms it often goes undiagnosed until a later stage.
The main reason stage 1 COPD symptoms go unnoticed is because according to GOLD guidelines, stage 1 COPD patients still have an FEV1 of 80% or higher.
A lot of times, patients can attribute their COPD symptoms to a few different things including:
- Smoking
- Old age
- Getting a cold
- Allergies
So rather than going to the doctor to see if anything is wrong, these symptoms get written off as something minor.
Symptoms

Stage 1 COPD only has a couple of different symptoms and they really aren't too severe:
- Minor airflow limitations
- Increase in mucus production
- Possible chronic cough
- Wheezing
- Fatigue sets in faster and easier
When you look at the list of stage 1 COPD symptoms, it's easy to see how they can can be attributed to having allergies, having a cold, or that they are just a part of getting older.
This is where it gets kind of tricky... You want to catch COPD as early as possible so you can start treating it immediately. However, COPD isn't the first thing that comes to mind when you think of coughing and getting fatigued faster.
So as you become aware of these symptoms you will want to talk with your doctor.
If you were a smoker or worked a job with a lot of exposure to lung irritants and pollutants you should be more vigilant when evaluating your own symptoms.
Treatment Options for Stage 1 COPD
If you are lucky enough to catch COPD in its earliest stage, you have the best odds to slow the progression of the disease and live a high quality life! At this point, your treatment plan is more of a preventative maintenance plan to reduce any risk of progression.
Your goal is to prevent the progression of the disease or prolong the progression of the disease.
That's not to say the disease won't progress, but you should have an easier time managing the disease and its symptoms.
After being diagnosed with stage 1 COPD, there are a few different treatment options you will utilize:
Short-Acting Bronchodilators

Because you were diagnosed with stage 1 COPD, your list of medications is going to be minimal. Depending on your personal situation, your doctor may or may not prescribe you a short-acting bronchodilator. It's usually the first medication prescribed to help you manage your COPD.
A short-acting bronchodilator's main purpose is to ease your COPD symptoms. Normally in stage 1 your symptoms come and go, but they aren't debilitating and often aren't that noticable. This is why many with stage 1 do not know they have COPD yet. Short-acting bronchodilators will come in handy whenever you feel your symptoms becoming more persistent.
When you get prescribed a bronchodilator there are a few different options your doctor may prescribe you:
- Anticholinergics (ipratropium)
- Beta2-agonists (albuterol or levalbuterol)
- A combination of the two (a combination of albuterol and ipratropium)
Vaccines
Vaccines play a vital role in treating COPD at every stage of the disease. While they aren't going to do anything to directly impact your lung function or your symptoms, for stage 1 COPD, vaccines will help protect you from viruses that could speed up the progression of your COPD and possibly put you in the hospital.
The two most important vaccines for COPD are the:
- Flu vaccine
- Pneumonia vaccine
When you have COPD, whether it's stage 1 or stage 4, you are more susceptible to getting sick. So, by getting vaccinated you are providing your immune system with an added layer of protection.
Both the flu and pneumonia can speed up the progression of your COPD. Sometimes, after getting sick, your new symptoms or your increased symptom severity can subside, and other times they can be permanent.
You will want to speak with your doctor about other vaccines that might benefit you.
Quit Smoking

Quitting smoking is hands down the best thing you can do for your COPD. If you continue to smoke after your initial diagnosis, you are only speeding up the progression of the disease...
It's not going to be easy, but nothing worth while is easy. I'm sure you have seen an infinite amount of articles on quitting smoking and the benefits of quitting so I'm not going to hammer them home right now.
Instead, here are a few great articles to help you successfully quit smoking:
Quitting Smoking: Why It's So Hard and How to Conquer the Habit
Getting Cigarette Smoke Out of Your Home and Car
13 Best Quit-Smoking Tips Ever
Avoid COPD Triggers

After being diagnosed with COPD, you want to do everything you can to avoid lung irritants, pollutants, and other COPD triggers.
Now, because you have stage 1 COPD, you might not be as sensitive to irritants and pollutants, but that doesn't mean you shouldn't avoid them. The more exposure to these irritants and pollutants that you have, the higher risk you have for aggravating your lungs and making your symptoms worse.
As a matter of fact, lung irritants and pollutants can be linked to the other 20% of diagnosed COPD patients.
Here is a list of known lung irritants you will want to avoid:
- Pollution
- Dust
- Pollen (if you suffer from allergies)
- Chemical based cleaning supplies
- Perfume/cologne
- Smoke
Click here to see a complete guide on COPD triggers, how to avoid them, and more!
Change Your Diet

One of the best things you can do for your overall health is; make healthy changes to your diet. Now before you go make any changes to your diet, make sure you speak with your doctor about any changes you want to make.
When you're battling COPD there are foods you want to avoid and foods you want to consume more of. And if you are diagnosed with stage 1 COPD, making these changes to your diet sooner rather than later will help slow the progression of the disease and it will help maintain your quality of life.
A healthy COPD diet is going to consist of:
- Lean protein
- Fruits
- Vegetables
- Whole grains
- Hydrating liquids
- Vitamin supplements
Some foods you want to avoid with COPD:
- Fried and processed foods
- Heavily spiced foods
- Caffeinated and sugary drinks
- Alcohol
- Salty food
- Nitrates
- Sulfites
- Food that causes heartburn, GERD, or acid reflux
For more information on nutrition for COPD, check out these great posts:
The Official Guide to COPD Nutrition
COPD Nutrition: Eating All of the Right Things
American Lung Association: Nutrition
Exercise and Stay Active

Exercising and staying active after being diagnosed with COPD can seem counter-productive... Why would you want to exert yourself when you already have a hard time breathing? But the fact of the matter is; exercising almost as important as quitting smoking.
By exercising and remaining active you will:
- Slow the progression of your COPD
- Improve oxygen delivery throughout your body
- Help your body use oxygen more efficiently
- Strengthen muscles around lungs to improve breathing
- Boost your energy levels
- Boost your immune system
There are a number of different ways you can exercise and remain active. So, whether you enjoy going to the gym or not, you should be able to find a way to exercise and remain active that you actually enjoy!
Here are a few different ways you can remain active:
- Hiking
- Gardening
- Yoga
- Golf
- Kayaking
- Playing an instrument
- Bowling
- Swimming
When it comes to remaining active, you want to do things you truly enjoy and require a little bit of physical activity. These are just a few options... The possibilities are endless. You just have to find the things you like to do!
As for exercising, you should consult your doctor to see how often you should be working out and what you can handle. But, just in case you were wondering, here is a list of some COPD friendly exercises :
- Walking
- Jogging
- Bicep curls
- Shoulder press
- Squats
- Lunges
- And many more
There are so many different ways you can exercise for COPD. You can workout at home, you go to the gym, or you can go to a park and enjoy the weather outside. It really doesn't matter where you workout, as long as you workout!
Because this topic is so broad, here are some great articles that will help you exercise with COPD:
The Official Guide to Exercising With COPD
59 Hacks and Tips You Can Use Immediately to Make Life With COPD More Manageable (Great tips to make working out at home as easy as possible)
ElderGym.com (Great online resource with videos to follow along as you workout)
Stage 1 COPD Overview
Stage 1 COPD is the least severe stage. Symptoms are barely noticeable and often times go untreated. Treatment options are more like preventative maintenance to slow the progression of the disease to further stages and to maintain your quality of life. You don't need supplemental oxygen with stage 1 COPD.
Your goal should be to make healthy lifestyle changes like quitting smoking, avoiding lung irritants, improving your diet, and exercising more.
Stage 2 COPD (Moderate)
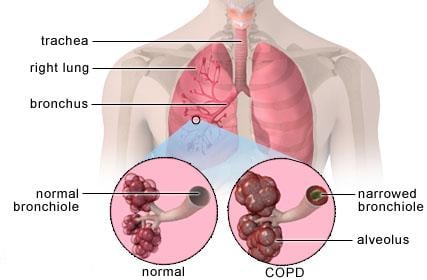
Although some people still ignore the warning signs, stage 2 COPD is typically when most patients really start to notice their symptoms and seek medical help.
As other symptoms become more prevalent with COPD, chances are your lung function is also declining. According to GOLD guidelines, stage 2 COPD patients have an FEV1 of 50-79%.
Symptoms
Stage 2 COPD symptoms are more severe and persistent than stage 1 symptoms. This is when symptoms are often noticed due to more severe symptoms. You may also experience more COPD symptoms, in addition to your original stage 1 symptoms:
- Increased breathlessness, especially after exertion
- Airflow limitations worsen
- Cough severity worsens and becomes more persistent
- Increased phlegm production
- Phlegm is harder to expel
The most significant difference between stage 1 and stage 2 COPD is the symptom severity and how often you experience your symptoms. Symptoms in stage 2 are typically too severe and persistent to ignore.
Treatment Options
Treatment options for stage 2 COPD are pretty similar to stage 1 COPD. However, your lifestyle changes become even more important as your COPD progresses.
With stage 2 COPD, your new treatment options will be used in addition to your stage 1 COPD treatment options.
Here are the treatment options for stage 2 COPD. Remember, these are in addition to your stage 1 COPD treatment options:
Long Acting Bronchodilators
With stage 1 COPD, you get prescribed a short acting bronchodilator to manage persistent symptoms. You will keep using your short acting bronchodilator as needed, however, your doctor may prescribe one or more long acting bronchodilators.
Long acting bronchodilators are used to treat COPD over a longer period of time. Instead of taking it as needed, like you do with the short acting bronchodilators, you will take your long acting bronchodilators 1 or 2 times a day as prescribed.
As you use the long acting bronchodilators you will prevent and reduce symptoms and gradually help ease your breathing.
According to Healthline.com here is a list of available long acting bronchodilators:
- Aclidinium (Tudorza)
- Arformoterol (Brovana)
- Formoterol (Foradil, Perforomist)
- Glycopyrrolate (Seebri Neohaler)
- Indacaterol (Arcapta)
- Olodaterol (Striverdi Respimat)
- Salmeterol (Serevent)
- Tiotropium (Spiriva)
- Umeclidinium (Incruse Ellipta)
Depending on your situation your doctor may prescribe you combination medications. Combination medications are typically a combination of two long acting bronchodilators or one corticosteroid and one long acting bronchodilator.
According to Healthline.com here is a list of available combination medications:
Combinations of two long-acting bronchodilators include:
- Glycopyrrolate/Formoterol (Bevespi Aerosphere)
- Glycopyrrolate/Indacaterol (Utibron Neohaler)
- Tiotropium/Olodaterol (Stiolto Respimat)
- Umeclidinium/Vilanterol (Anoro Ellipta)
Combinations of an inhaled corticosteroid and a long-acting bronchodilator include:
- Budesonide/Formoterol (Symbicort)
- Fluticasone/Salmeterol (Advair)
- Fluticasone/Vilanterol (Breo Ellipta)
Pulmonary Rehabilitation
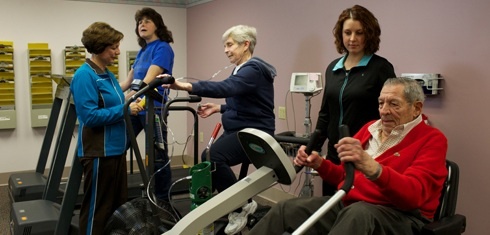
Due to the decline in lung function from stage 1 COPD to stage 2, your doctor may recommend that you enroll in a pulmonary rehabilitation program.
Don't think of this as a bad thing...
Pulmonary rehab can change your life for the best!
In short, pulmonary rehab is an extensive "training" program that teaches you how to cope with your respiratory disease, how to manage your symptoms, and how to implement new changes into your life that will help your overall health.
Patient Education

Education plays a crucial role in successfully treating and managing COPD. In pulmonary rehab you are going to get an educational boot camp, but it won't be torturous like an actual boot camp.
You will cover a wide range of topics during your educational sessions. Here are some of the topics you will cover:
- Coping skills
- Healthy diet
- Treatment adherence
- COPD friendly exercises
- Inhaler techniques
- Breathing exercises
- Support groups
Don't worry, your pulmonary rehab won't be filled with a bunch of "classroom" sessions. You will be partaking in physical activities, group discussions, and more! All of this knowledge can later be used at home to continue pulmonary rehab at home.
Diet and Exercise with Pulmonary Rehab
There are very few things that will be as beneficial as making changes to your diet and exercise routines. In your pulmonary rehab program you will not only learn what will benefit you the most, but why it will benefit you.
There's nothing like being told to do something without an explanation as to why... So here's what you can expect to learn from the diet and exercise portion of your pulmonary rehab program:
- How to properly exercise for your COPD and why
- How often you should workout
- How to use your breathing techniques while exercising
- Which foods can cause problems with your COPD and why
- How often you should eat small meals
- Tips to make preparing meals easier
- And much more!
You should have peace of mind knowing that your pulmonary rehab program will prepare you to make these changes stick in your routine even after you've completed your rehabilitation!
Support Groups

Having a strong support system around you while you're battling COPD makes a huge difference. And with your pulmonary rehab program, you have one of the best support groups around!
You have some people you can relate to and confide in. You have people who have been through the same thing you are currently going through. You have people who need your support as they go through the same stuff you already went through.
While you're in your rehab program you will have support group sessions where you can talk about the victories you've accomplished in class and at home, the downfalls you've had to deal with, and anything you may be going through.
Not only will you have fellow COPDers in your group, but you will have access to medical professionals every step of the way!
This is one huge advantage pulmonary rehab provides you with that other support groups may not be able to offer!
As your pulmonary rehab program comes to a close, chances are you made a couple new friends!
Depending on where you're located, you might have some people in your program that live close to you.
It would be really beneficial to stay in contact with the people you meet so you can keep your support group and try to hold each other accountable!
Don't just keep the friendship going for support and accountability either... Go out and do things you enjoy together!
Click here to find a pulmonary rehab program near you!
Antibiotics/Corticosteroids (Inhaled or Oral)

Depending on your symptom severity and if you have an infection, your doctor may start to prescribe antibiotics to help treat and manage your COPD.
Also, stage 2 COPD is when you may start experiencing COPD exacerbations.
For the most part, you will be prescribed antibiotics when you are sick with a bacterial infection. Especially if the infection can lead to a COPD exacerbation.
If your infection is viral, antibiotics won't be effective. However, your doctor will prescribe you medicine to help boost your immune system and to manage your symptoms.
If you experience an exacerbation, your doctor will prescribe you a regiment with antibiotics and corticosteroids to help you recover as soon as possible!
Here is a list of some of the medications you may get prescribed if you suffer from an exacerbation:
- Fluticasone (Flovent HFA, Flonase, others)
- Prednisone
Although there aren't any long-term antibiotics on the market for COPD, researchers are consistently looking for ways to better treat COPD.
In one case study, researchers found that Azithromycin reduced COPD exacerbation frequency by 20%!
Azithromycin hasn't been fully approved for this use, but your doctor may prescribe it to you if they think it will be beneficial.
Stage 2 COPD Overview
Stage 2 COPD is the stage where most patients can no longer ignore the symptoms and seek medical help.
Treatment options have become more intense and are more about managing symptoms rather than preventative maintenance. Your treatment will include methods from stage 1 and stage 2.
Your breathing might begin to suffer even when doing simple tasks. However, you probably don't need oxygen at this point. And if you do, it's not 24/7 oxygen therapy.
Your goals should be to continue making healthy lifestyle changes and to monitor your symptoms.
COPD Stage 3 (Severe)
At stage 3 COPD, symptoms are far too debilitating to ignore any longer. Along with the common COPD symptoms you may begin to experience more advanced symptoms that indicate your COPD is more severe. And according to GOLD guidelines, stage 3 COPD patients have an FEV1 of 30-49%.
Symptoms
With stage 3 COPD, the symptoms are too severe to go without medical help. Not only do you experience more advanced symptoms in stage 3, but your previous symptoms are increasingly more prominent and harder to manage.
Along with previous symptoms, here are some of the symptoms you may experience with stage 3 COPD:
- Increased breathlessness
- Increase in COPD exacerbations
- Serious difficulty with any physical activity
- Even more fatigue
- Morning headaches
- Edema (swelling around your feet or ankles)
- Trouble with your weight (hard to maintain, lose, or gain weight)
Along with a few added symptoms, the biggest difference between stage 2 and stage 3 COPD symptoms is the severity and frequency.
At stage 3, your symptoms have become more advanced and they require more attention to ensure your treatment program is working.
Treatment Options

Stage 3 COPD treatment becomes a little more intense than with previous stages. This is partly because your symptoms are more persistent and harder to manage. Your treatment goal is to keep your symptoms at a manageable level and to prevent loss of quality of life.
Along with treatment methods for stage 1 and stage 2 COPD, here's what your doctor may recommend for stage 3:
More Frequent Pulmonary Function Tests
To ensure you're following your treatment plan and that your treatment plan is working your doctor will request that you see each other more often to do a pulmonary function test and to check up on you.
You and your doctor will discuss your situation to determine how you've been feeling, see what you feel is working, and to see if there is anything that can be done differently to benefit you.
Along with your typical conversation, your doctor is going to want to run more pulmonary function tests to be absolutely positive your treatment is doing its job! The results of the test will tell your doctor how fast your COPD is progressing and how he or she should adjust your treatment.
Avoid Lung Irritants and Pollutants
As your COPD progresses it becomes more and more important to avoid lung irritants and pollutants. It's nearly impossible to completely avoid them, so you will have to do the best you can.
Here is a list of some common lung irritants:
- Smoke (cigarette smoke, smoke from a fire, smoke from a BBQ, etc.)
- Environmental pollution
- Allergens
- Perfume/cologne
- Chemical based cleaners
- Aerosol sprays (Lysol, Febreeze)
- Air Fresheners
- Dust
- Extreme weather conditions
You're not going to be able to control what other people wear in public or if someone is allowed to smoke in a certain area outside. What you can do is prepare yourself for a situation like that arising.
If you're going to be in public here are a couple of precautions you should take:
- Keep an N95 face mask with you whenever you go in public. This will protect you from lung irritants you simply cant avoid. Not to mention it will come in handy during cold/flu season
- Check air quality reports before you leave the house. If the air quality is anything but good or moderate, it's best to stay indoors. You can view your local air quality here!
- If you suffer from allergies, it's important to check the allergen report in your area to prevent exposure to your specific allergens. You can view your local allergen report here!
For more tips on how to avoid lung irritants click here!
Vaccinate and Avoid Large Crowds

We already talked about getting vaccinated for COPD during this post, but you should be doing this every year whether you have stage 1 COPD or stage 4 COPD just to protect yourself.
As your COPD progresses you may want to avoid large crowds, especially during cold and flu season.
This will minimize your risk of catching a cold, the flu, or pneumonia and it will lower your risk of experiencing an exacerbation.
Even though you got vaccinated, there are quite a few people who refuse to get vaccinated. Not to mention there is no vaccine for the common cold. So, it can get increasingly difficult to protect yourself in a large crowd.
However, if you absolutely have to go out and there is a large crowd, here are a few things you can do to protect yourself:
- Wear an N95 rated mask
- Wash your hands frequently
- Carry disinfecting wipes to clean commonly touched items like shopping carts, door handles, public tables, etc. before you use them
Supplemental Oxygen Therapy
Depending on your situation, you may have been prescribed oxygen at an earlier stage. However, oxygen therapy is not designated for any specific stage of COPD. Your need for oxygen therapy depends on your SPO2 levels.
As your COPD becomes more severe and your lung function deteriorates there's a good chance you are going to require supplemental oxygen therapy.
When it comes to oxygen therapy for COPD, a lot of patients look at it as a burden rather than a helpful tool. Supplemental oxygen is extremely beneficial and should never be looked at as a punishment.
Here are just a few of the many benefits of supplemental oxygen for COPD:
- Prolongs your life
- Improves quality of life
- Relieve breathlessness
- Lessens fatigue throughout the day
- Improves exercise capacity and performance
- Improves sexual performance
- Can prevent morning headaches
- Helps slow or prevent heart failure
When you get prescribed oxygen, chances are you will get setup with a home oxygen concentrator and then you will have some sort of portable oxygen equipment.
While home oxygen concentrators have basically become an industry standard, you have a few different options when it comes to equipment:
Portable Oxygen Concentrators

When it comes to portable oxygen therapy, portable oxygen concentrators are the future. They are FAA approved, battery operated machines that can produce their own medical grade oxygen.
Rather than requiring someone to refill a concentrator or bring you a new one every couple weeks, these machines draw in ambient air, send it through a filtration process to produce medical grade oxygen.
There are a handful of options to choose from with portable oxygen concentrators. There are units as light as 2 pounds and they go up to 20 pounds.
The smaller and lighter units are pulse flow only, whereas, the units that are 10 pounds or more are continuous flow units.
The reason why continuous flow units are bigger and heavier is because they need a larger motor and compressor to produce that much oxygen.
However, the size of the continuous flow units should not intimidate you or be a deal breaker. In a lot of cases, it can take less energy to pull a 20 pound concentrator behind you than it does to carry a 5 pound concentrator.
You can read more about that here!
When it comes to choosing a portable oxygen concentrator for yourself or a loved one, you want to make sure the unit is going to actually work. If the machine cannot supply enough oxygen, it is not a good fit.
To help make your research a little easier, here are a couple of great articles that will help educate you on the different makes and models!
How to Compare Portable Oxygen Concentrators Like an Expert
Best Portable Oxygen Concentrators of 2016-2017
If you don't know much about portable oxygen concentrators, we also have a downloadable guide that will tell you everything you need to know! You can download it here:
Liquid Oxygen

Liquid oxygen is one of the more popular choices for insurance and medicare to supply to patients. With liquid oxygen, you will rely on your oxygen provider to drop tanks off on a regular basis. Or they will drop off a large liquid oxygen reservoir to store in your house so you can refill your own bottles as needed.
Liquid oxygen tends to last longer than standard oxygen tanks, but they still carry the same risks.
They are flammable so they can explode, you cannot take them on an airplane, and the process of getting them refilled can be cumbersome.
With that being said, there are a ton of oxygen patients out there who absolutely love their liquid oxygen. And there are a lot of patients who simply can't use a portable oxygen concentrator because none of the models can supply them with enough oxygen.
There's really no "best portable oxygen delivery system" because you need to find what works best for you.
Supplemental Oxygen Tanks

Supplemental oxygen tanks seem to be the standard issued oxygen equipment. They certainly get the job done, but they require a decent amount of upkeep from your oxygen provider.
You will rely on your oxygen supplier to bring you new tanks on a regular basis and they will pick up your old tanks to reuse. So your supply may be limited compared to a liquid oxygen reservoir or a portable oxygen concentrator.
Supplemental tanks come in a wide variety of sizes. Some bottles are small enough to carry and others require a cart to transport them around.
Some people prefer supplemental tanks over liquid oxygen or portable oxygen concentrators which is understandable.
If it isn't broken, don't fix it, right? Just like with liquid oxygen, a lot of patients also stick to tanks because they simply cannot use a portable oxygen concentrator.
Before you make your oxygen decision, make sure you do your research and find the device or system that will help you live an active life.
Stage 3 COPD Overview
Stage 3 COPD is the stage where symptoms become more severe, difficult to manage, and more persistent.
Your treatment options have become more intense and you have to closely monitor your symptoms. Your doctor may try switching treatment methods up to see if there's a more effective way to manage your COPD.
You might experience more advanced symptoms like morning headaches and edema. Supplemental oxygen is more than likely being used at night and possibly 24/7.
Your goals at stage 3 should be to slow the progression of your disease through a strict treatment regiment and healthy lifestyle changes.
COPD Stage 4 (Very Severe)

Stage 4 COPD... Where do we even begin?
First of all, we see a lot of people, companies, and organizations referring to stage 4 COPD as "end-stage COPD". Well that is super comforting to hear...
Just kidding, that is probably one of the scariest things you can hear someone say when they are talking about your health.
No one wants to hear anything referred to as "end-stage" unless you're running a marathon and you are at the last stage of the race. It's discouraging, scary, and as far as COPD is concerned, it's just wrong.
There are many people living a high quality life for YEARS with stage 4 COPD. Take a look at the COPD Athlete Russell Winwood... That man does more than 95% of people without COPD.
Yes, things get more difficult during stage 4. Yes, you are more prone to getting sick or experiencing an exacerbation. And yes, your FEV1 is below 30%.
But none of that means you are at the "end-stage".
It's actually pretty ironic that stage 4 COPD would be referred to as end-stage COPD when all of the literature out there says a positive attitude can make a big difference in how you feel.
Alright, now that we have clarified that misconception about stage 4 COPD we can continue with the blog post.
Symptoms

During stage 4, you might only develop a few new symptoms. For the most part your symptom severity increases and it gets harder to recover from exacerbations.
So, along with the symptoms from the previous three stages, you may experience the following symptoms when you reach stage 4:
- FEV1 below 30%
- Significant airflow obstructions
- Chest tightness
- Pain near your chest or abdomen
- Trouble maintaining a healthy weight
- Heart problems from low O2 levels
- Depression
- Drowsiness
- Confusion
- Disorientation
- More frequent exacerbations
It's important to remember that everyone is different and you might not experience the same symptoms as the next person. The main indicator for the different stages of COPD is your FEV1 test results.
Treatment Options
Treating stage 4 COPD requires more effort and accountability. You really want to follow a strict treatment plan that includes:
- A strict and healthy diet
- A regular exercise plan
- Taking your medications properly (at the right time and in the correct order)
- Having a healthy support group
- Pulmonary rehab (if possible)
- A COPD action plan
To hold yourself accountable and to ensure you are following your doctor's treatment plan, we already have 59 hacks and tips you can use! You can view all of the hacks and tips here: 59 COPD Hacks and Tips
You are probably going to have more doctor's appointments when you have stage 4 COPD to ensure your treatment is working the way it is supposed to.
This will give your doctor the chance to make quick changes to your treatment plan to help you better manage your symptoms.
The treatment options for stage 4 COPD include everything from the previous stages, but you now might be eligible for lung surgery or a lung transplant.
Lung Surgery
Along with a stricter treatment plan with stage 4 COPD your doctor may decide that you will benefit from a lung volume reduction surgery or a complete lung transplant.
Typically, a volume reduction surgery or a transplant is a last resort because of the risk that can be involved.
Lung Volume Reduction Surgery
A lung volume reduction surgery (LVRS) is exactly what it sounds like, your lung volume gets reduced. Basically what happens is; your surgeon will go in and remove up to 30% of the diseased tissue.
You might be wondering, what does removing diseased tissue do? Well, there are a number of different benefits:
- Increased ability to exercise
- Fewer symptoms
- Fewer exacerbations
- Gives your healthy lung tissue more room to make it easier to breathe
Lung volume reduction surgery is not for everyone though. There are certain criteria that you need to meet in order to be eligible for this surgery.
However, the criteria is subjective and if your doctor feels you will benefit from it, you might get the green light if you don't meet all of the criteria.
Even though the criteria is subjective, we figured you might want to know what makes a "good candidate" for lung volume reduction surgery.
According to WebMD, people who meet the following criteria would be a good candidate for LVRS:
- Have severe emphysema that does not respond to medical therapy.
- Are younger than 75 to 80 years old.
- Have not smoked for at least 4 months.
- Have reasonable expectations of surgery results.
- Have areas of the lung that can be targeted.
- Have severe difficulty breathing, as determined by breathing tests.
LVRS is not a cure, but it can significantly improve your quality of life and make your COPD easier to manage.
LVRS is a really complex topic and it could have its own article. For more information on LVRS and to see if it would work for you check these articles out:
Lung Volume Reduction Surgery - Cleveland Clinic
Lung Volume Reduction Surgery Topic Overview - WebMD
Lung Volume Reduction Surgery for Emphysema - USC Keck School of Medicine
Complete Lung Transplant
A complete lung transplant is usually a last resort. There are common complications that can make a transplant very difficult, however it can add years onto your life and reduce your symptoms.
Normally, the procedure is recommended when you might not live without it. Or it's recommended when your disease is so severe you can no longer enjoy your life.
However, even if you fit one of those two groups of people, there are other criteria you have to meet in order to be eligible for a lung transplant:
- Have severe COPD
- Be under 65 years old
- Have stopped smoking
- Have family and friends who will help and encourage them during and after the surgery
- Be physically capable of undergoing surgery, follow-up medical treatment and participation in a pulmonary rehabilitation group
- Not currently have a drug or alcohol abuse problem
So, the criteria for a lung transplant are pretty strict, but that's only because there aren't always enough organs donated.
Complete lung transplants are extremely complex and while the benefits of a successful transplant are amazing, it's important to know the risks associated with a transplant:
- Organ rejection
- Bleeding and blood clots
- Cancer and malignancies due to immunosuppressants
- Diabetes
- Kidney damage
- Stomach problems
- Thinning of your bones (osteoporosis)
For more information on lung transplants check out these articles:
Lung Transplant Surgery - WebMD
Managing COPD: Lung Transplants - LungChicago
Stage 4 COPD Overview
Stage 4 COPD is the most severe stage. Your symptoms are extremely persistent and they are difficult to manage. But the most difficult thing about stage 4 COPD is the stigma around it.
It shouldn't be referred to as end-stage. There's no time line that says if you develop stage 4 COPD you only have a certain amount of time left. There's really no way to gauge that at any stage.
And that's not something you should really focus on, as it is different for every individual.
Do not let the fact that you have stage 4 COPD define your life. With proper treatment adherence and a strong support system you will be able to live a high quality life.
It won't be an easy battle, but it will be worth it!
Conclusion
As of right now, the 4 stages of COPD are defined by your FEV1 results. As your lung function declines, your COPD becomes more severe.
However, new research has come out that is putting an emphasis on symptom severity and quality of life instead of FEV1 results.
At each stage of the disease, you may begin to experience more symptoms and your symptoms may get harder to manage. Your treatment plan will also become more intense as your lung function declines.
Regardless of which stage you are in, there are ways for you to slow the progression of your COPD. By following your treatment plan, avoiding lung irritants, and having a solid line of communication with your care team you can live a high quality life for years to come!
To help your battle with COPD and to help slow the progression of your disease, we teamed up with nutritionist and best-selling author Kellie Hill to create a COPD meal plan. You can download it for free here!





