COPD exacerbations and flare-ups are taxing on both you and the healthcare system. Not to mention, they are one of the terrifying aspects of dealing with Chronic Obstructive Pulmonary Disease, and for a good reason. COPD exacerbations result in more than 100,000 deaths and over 500,000 hospitalizations each year. Did you know that within 30 days of hospitalization 21% of COPD patients will be readmitted to the hospital?
Imagine if you could make one simple change to your daily life that would reduce your chances of having a COPD exacerbation.
Or even better:
What if there were 13 simple changes and each of them can reduce your chances and they may even prevent exacerbations? Would you be interested to know what they were?
That’s exactly what we are going to share with you today in this post:
13 simple strategies that you can use to reduce your chances of experiencing and even prevent COPD exacerbations TODAY.
Table of Contents (Click one of the links below to go to that section of the post)
1. Pulmonary Rehab
2. Hydration is Key
3. Wash Your Hands Regularly
4. Reduce Indoor Air Pollution
5. Weather and Air Quality Reports Are Your Best Friends
6. Clean Your Home or Have Your Home Cleaned Regularly
7. A Fingertip Pulse Oximeter is a Necessity
8. Create a COPD Action Plan
9. Stay On Top of Medications and Vaccines
10. Dieting Makes a Huge Difference
11. Vitamin D
12. Regular Exercise for the Win
13. Get More Sleep
1. Pulmonary Rehabilitation
Visualize a COPD support group that offers education along with exercise sessions to help you adjust to life with COPD. That’s exactly what pulmonary rehab is. Pulmonary rehabilitation is one of the most important pieces to the puzzle when you have been diagnosed with COPD. In a controlled environment pulmonary rehabilitation gives you the courage to live an active, fun, and healthy lifestyle while managing your COPD exacerbations.
For starters, you will be in a group setting with other people diagnosed with COPD along with medical professionals who will educate you about your lungs and COPD. More importantly they will teach you little tricks to help ease some of those terrible COPD symptoms. There are several different components that make up a full pulmonary rehab course, these include but are not limited to:
- Educational sessions discussing: breathing techniques, exercise techniques, disease processes, respiratory medications, and oxygen therapy
- Exercise reconditioning sessions
- Nutrition education
- Energy conservation techniques
- Oxygen dosing (when applicable)
- Individualized counseling reviewing results of tests, program recommendations, exercise prescription, offered by a medical professional will answer any questions you may have

A standard pulmonary rehab program lasts six to ten weeks to ensure you are ready to treat and manage your COPD on your own. Most patients say pulmonary rehab was a key element to living a better life with COPD. Everyone we have spoken with has highly recommended other patients to go!
The first step to getting started with pulmonary rehab is to find a program. Here are a few different links for you to use to locate a program close to home:
- COPD Foundation
- Emphysema.net
- American Lung Association
- Local.com (search for pulmonary rehabilitation)
Joining a pulmonary rehab program yields immediate benefits. While you may be meeting with the group weekly, you will be responsible for keeping up with the program while you are at home to stay in tip top shape for the next session.
Upon completion of the pulmonary rehab program you will be equipped with all the necessary tools to treat and manage the progression of your COPD and it will enhance the following 12 tips in this post! Not to mention, by following the pulmonary rehab program you can essentially minimize the amount and severity of exacerbations you may experience.
Click Here to Go Back To The Top2. Hydration is Key

When treating and managing your COPD it is imperative that you drink plenty of fluids. Staying hydrated can make an enormous difference in your COPD, but there are some recommended guidelines to follow.
When we say drink plenty of fluids, we mean caffeine-free liquids with as little sugar as possible. While the sugary and caffeinated drinks are tasty, they can dehydrate you and cause problems like bloating which can make it harder for you to breathe.
Obviously, water is the top fluid for hydration, but why is it so important to stay hydrated with COPD?
Your immune system runs at its highest ability when you have proper nutrition and proper hydration. You will be giving your immune system a much-needed boost by staying hydrated. Hydration will help prevent you from getting sick or experiencing more or worse COPD exacerbations. Proper hydration is especially important given that supplemental oxygen may dry your mucus membranes and cause irritation.
Staying hydrated also thins your mucus making it much easier for you to expel from your body.
It is recommended that you drink 64 to 86 ounces of caffeine-free liquids every day. That equals 8 to 12 cups. Here are the best fluids for staying hydrated:
- Water
- Real Fruit Juice (with little to no added sugar)
- Decaf Coffee
- Decaf Tea
- Milk
It may be hard to cut out some of your favorite drinks like soda, but it’s important to do the best job you can to take care of yourself. Yes, you can treat yourself to a soda every now and then, but make sure to follow it up with a glass of water or two so your soda doesn’t dehydrate you. If you need some ideas or tricks on how to drink more water every day, click here.
Click Here to Go Back To The Top3. Wash Your Hands Regularly
Getting sick plays a major role in experiencing COPD exacerbations. Something as small as a minor head cold can wreak havoc on your ability to breathe and your immune system. Having a hard time breathing and a compromised immune system can easily cause a COPD exacerbation.
As you touch different surfaces and objects throughout the day germs begin to build-up on your hands. As the germs accumulate you can infect yourself by touching your eyes, nose, and/or mouth.
While it is impossible for you to keep your hands germ-free, frequently and regularly washing your hands is easily one of the best ways to reduce your chances of experiencing an exacerbation from getting sick.
Washing your hands takes a little more work than just putting your hands under running water. Here is a step-by-step process on how to properly wash your hands from the Mayo Clinic:
- Wet your hands with running water – either with warm or cold water
- Apply liquid, bar, or powdered soap
- Lather well
- Rub your hands vigorously for at least 20 seconds. Remember to scrub all surfaces, including the backs of your hands, wrists, between your fingers, and under your finger nails.
- Rinse well
- Dry your hands with a clean or disposable towel or air dryer
- If possible, use a towel or your elbow to turn off the faucet
Now that you know how to properly wash your hands, it’s time to determine when you should wash your hands, aside from when they look dirty.
Always wash your hands before any of the following activities:
- Preparing food
- Eating
- Treating wounds
- Giving medicine
- Caring for a sick or injured person
Always wash your hands after any of the following activities:
- Preparing food, especially raw meat or poultry
- Using the toilet
- Changing a diaper
- Touching an animal, animal toys, leashes, or waste
- Blowing your nose
- Coughing/sneezing into your hands
- Treating wounds
- Caring for a sick person
- Handling garbage
- Using chemically based cleaners
- Utilizing garden chemicals
- Shaking hands with others
When washing your hands, keep in mind that regular soap will do the job just as well as antibacterial soap. In fact, using antibacterial soap may lead to the development of bacteria that are resistant to the soap’s antibacterial agents. It’s also important to remember that washing your hands with soap and water instead of using hand sanitizer is better for your immune system. Using hand sanitizer kills 99.9% of germs including the good ones, but it will work in a pinch if you can’t get to a sink.
Click Here to Go Back To The Top4. Reduce Indoor Air Pollution

Keeping your home free of indoor pollutants can vastly improve your quality of life while minimizing the amount of exacerbations you may experience throughout the year. The amount of indoor pollutants that could be in your house may surprise you. Fear not, most are quick and easy fixes. Here is a list of indoor pollutants:
- Dust
- Mold
- Mildew
- Chemicals from cleaners and air fresheners
- Fumes from perfumes, colognes, and hairspray
- Pet dander
- Humidity
- Smoke from cigarettes, fires, cooking, and wood-burning stoves
There are many different things you can do and strategies you can use to reduce and even eliminate the amount of indoor pollutants you are exposed to.
Dealing With Dust
Dust can cause a flare-up of symptoms in a heartbeat, especially if you suffer from allergies. By keeping your home as dust free as possible you will improve the quality of air that you breathe and reduce your chances of experiencing an exacerbation. Here are a few tips on how to make your house as dust free as possible and maintain that level of cleanliness:
- Dust surfaces regularly to prevent buildup
- Get air ducts cleaned periodically
- Clean or replace air filters at least twice per year
- Cover mattress, box spring, and pillows in dust-mite resistant covers
- Wash sheets, blankets and pillow cases once a week in hot water (at least 131 degrees Fahrenheit)
- Eliminate dust collecting décor like stuffed animals and decorative items
- Remove piles of magazines and books (they degrade overtime and produce more dust)
- Use fewer textiles like throw blankets, pillows, and tablecloths as they can produce and trap dust
- Pay attention to seasonal allergies and keep windows closed when allergen counts are high or high winds are anticipated
- Have friends, family, and all guests take off dirty shoes at the door
- Vacuum carpets regularly (twice per week if possible)
- If practical/within your budget replace carpeting with wood floors

If possible, it’s best to have someone clean for you or help you clean. For one, cleaning can take a lot of energy and leave you feeling short of breath. Also, when you vacuum and dust you are exposing yourself to a lot of dust that gets kicked up in the act of cleaning. By reducing your contact with the dust particles you’re keeping your lungs as healthy as possible.
We recommend choosing cleaning products that are hypoallergenic. To dust, you might want to consider the new Clorox Triple Action Dust Wipes these are excellent for dust, hair, and allergens. Or, try Hypo-Allergenic Dusting and Cleaning Spray by Endust which is formulated with less-irritating ingredients and free of perfumes and fragrances that could trigger COPD expirations. Continue reading for our recommendations of organic cleaning solutions.
Eliminating Fumes
As you know, being exposed to fumes, scents, and smoke throughout the day can really cause problems with your COPD. In fact, if you are sensitive to strong scents or fumes and happen to inhale them you may experience chest tightness and shortness of breath almost immediately. Eliminating fumes from your home is much less work than making your home dust free. Here are some tips on how to eliminate strong scents and fumes from your home:
- Replace chemically based cleaners, especially those with bleach or ammonia, with “green” cleaning supplies, soap and water, baking soda, or vinegar
- If you can’t replace your cleaning products, have someone else do the cleaning for you to avoid the harmful fumes
- If you don’t have someone that can help you clean, the COPD Foundation recommends wearing a respirator mask rated “N95” by the National Institute for Occupational Safety and Health
- Use unscented shampoo, soap, deodorant, and hair spray
- Avoid cigarettes at all costs
- Avoid using wood burning fire places and stoves, the smoke produced can cause complications with your COPD
- Keep your home properly ventilated
- Use an air purifier with a HEPA filter
Once you start making changes in your home and eliminate the fumes, scents, and smoke that irritates your lungs you will immediately notice a difference in how your feel. It will also be easier for you to control your symptoms.
Controlling Humidity

Living in areas with high humidity can make it harder for you to breathe and possibly trigger an exacerbation, especially when the humidity invades your home. Low humidity areas are ideal for COPD patients like yourself, with 40% humidity being the sweet spot. You can easily and accurately check the humidity levels in your house with this inexpensive humidity monitor from Amazon.
Unfortunately, you can’t do anything to reduce the humidity outdoors, aside from moving, but you can and absolutely should control the humidity levels in your house. The steps you take to do so will be dependent on the weather outside. In order to control the humidity levels in your house, follow these tips:
- Watch the weather index to get an idea of how humid it is going to be that day
- Properly ventilate your home, especially areas that create moisture like the kitchen, laundry room, and bathroom
- Use fans to increase ventilation
- Take colder, shorter showers
- Open or close your windows based on the humidity and temperature outside
- Use a dehumidifier to reduce humidity
- Use a humidifier to increase humidity
- Adjusting the AC or heat also helps control humidity levels
Moisture Breeds Bacteria
Moisture build up may go unnoticed until it’s too late and your symptoms start to flare-up. Simply put, moisture breeds bacteria, mold, and mildew which can reduce air quality and can be detrimental to managing your COPD. By following these simple steps, you can nip moisture build up in the bud and improve the air quality in your home right now:
- Repair all leaks that may be present
- Immediately wipe up spills
- Use fans to increase ventilation in kitchens and bathrooms
- Replace sponges frequently
- Clean or replace showerheads at least twice per year
- Throw out water damaged carpet or cushions
5. Weather and Air Quality Reports Are Your Best Friends
Staying up-to-date on weather, pollen, and pollution reports can save you from a terrible COPD exacerbation. There are a few important factors to be mindful of, especially if you also suffer from asthma. Extreme temperatures, high pollen counts, and high pollution counts have all been known to cause COPD symptoms to flare-up and possibly cause hospitalization.
With these tips you will know what to look for, how to prevent yourself from getting exposed to the elements, and how to prepare yourself if you absolutely have to go outside when the tables are turned against you.
Extreme Temperatures and Weather Conditions

Dealing with extreme temperatures can be frustrating for anyone. Depending on where you live, extreme temperatures are present for almost half of the year. During the summer months extreme heat and humidity, with some areas regularly breaching triple digit temperatures, are a concern. During the winter you might be subjected to frigid temperatures and strong winds.
With a few exceptions to the rule, hot and humid climates cause COPD symptoms to flare-up. There are a select few people with COPD who do better in humid weather. Hotter temperatures also usually lead to higher pollution counts and lower air quality scores. Here are a few tips to help you beat the heat and manage your COPD symptoms during the summer:
- Check weather reports daily
- Stay inside an air-conditioned environment on the hottest and most humid days
- Limit activities to stay cool
- If you must go outside, go when the temperature is as mild as possible (preferably in the morning or the evening)
- Stay hydrated and drink a lot of water, not only does it help thin mucus and boost your immune system, but it will also help regulate your body temperature
When the weather gets cold and windy, COPD symptoms are tough to manage. In fact, cold weather and strong winds are known to be COPD exacerbation triggers. Cold temperatures can also cause you to be fatigued even if you haven’t had to exert yourself. Here are some tips that will help you reduce exacerbations in the winter:
- Avoid going outside in the extreme cold
- Avoid going outside when it’s really windy
- When you go outside wear a loosely worn scarf or face mask over your nose and mouth
- Breathe in through your nose when outside, this warms the air up before it reaches your lungs
- Keep your oxygen tubing inside your clothing to warm the air
- Wear several layers of loose clothing to protect you from the cold without restricting your breathing
- Keep your inhalers warm as their optimum operating temperatures range between 50 and 80 degrees Fahrenheit
Air Quality Is Key

As we mentioned before, COPD and air quality go hand in hand. Environmental pollution is one of the leading risk factors of COPD for non-smokers. When you expose yourself to high levels of pollution you are putting yourself at risk of experiencing an exacerbation. Depending on where you live, it may be harder to completely avoid pollution, especially in a major city like Los Angeles or New York. However, if you take these tips and apply them to your everyday life you will be able to minimize your exposure:
- Regularly check the air quality index which can be found here
- Watch the news or read the paper to get warnings on pollution levels in your area
- Follow advice from public service announcements telling you what level of outdoor activity is okay
- Avoid poor air and harmful fumes when traveling by car
- Take alternate, less crowded routes to your destination during rush hour
- Plan your travel when traffic is light
- Travel with your air conditioning on and windows rolled up (keep one window cracked to prevent oxygen from accumulating while you are traveling)
- Stay indoors when air quality reports are poor
- Keep windows closed and air conditioning on in your home on high pollution days
Pollution isn’t the only thing that can affect the air quality for COPD patients. If you suffer from allergies it’s important to watch pollen counts for your area because allergies can cause your symptoms to flare-up in no time. Although there are several over-the-counter allergy medicines available, there are several different things you can do to prevent your allergies from affecting your COPD.
- You should check the allergy forecast for your area every day. It can be viewed here
- If the allergy forecast is medium-high you will want to stay inside and keep your windows and doors closed and your air-conditioning unit on
- Check with your doctor to see what allergy meds are okay for you to take
- Regularly clean or have someone clean your house to prevent dust and pet dander from building up
- Have your pet, if they go outdoors, brushed regularly as they are known to bring dust, dirt, and pollen into your home
- If you must go outside when the allergy forecast is not favorable, carry your inhaler with you
6. Clean Your Home or Have Your Home Cleaned Regularly

Having a clean household can make a big difference when it comes to managing your COPD and preventing exacerbations. Indoor air pollutants are a major risk factor for exacerbations and will make it extremely hard to effectively manage your disease.
Indoor air pollution comes from various sources including, but not limited to; wood burning stoves, wood burning fireplaces, dust build up, pet dander, chemically based cleaners, perfume, and cologne. Don’t be intimidated by the long list of pollutants, we will go over how to minimize your exposure and offer alternative methods and products that will be COPD friendly.
First and foremost, if it’s feasible for you to do so, hire a service or ask a family member to clean for you. Not only do you have to worry about dust, fumes, and your COPD but cleaning with COPD requires a lot of energy and planning. There are services like Molly Maid, Merry Maids, and Maid Brigade that will come out to your house and clean on a regular basis.
If hiring a maid service isn’t an option, consider asking your children or grandchildren to clean for you or help you clean. After the original deep cleaning it will just need to be maintained which shouldn’t be too much to ask of loving family members. The list of cleaning duties would include:
- Dust all surfaces often, including lampshades and windowsills with a damp cloth
- Vacuum weekly with allergen-proof vacuum bags (you may also wear a mask for extra protection)
- Wiping down and disinfecting countertops
- Keep bathrooms clean and dry
- Laundry
- Washing dishes
If a cleaning service isn’t an option and you don’t have family nearby it’s important that you clean regularly within your means. Before we can get into a regular cleaning schedule we need to go over some quick tips that will help reduce indoor air pollution before the cleaning even starts.
Get Your Air Ducts Cleaned Periodically
Hiring a professional duct cleaning service will drastically increase the air quality in your home depending on the last time you got them cleaned. According to the EPA, if there is substantial visible mold growth, the ducts have an infestation of insects or rodents, or if the ducts are excessively clogged and are releasing particles into the home then you should have this cleaning done right away.
Make sure your professional duct cleaning service cleans all of the duct system. If they do not, your ducts will become re-contaminated almost immediately. If you have a furnace, stove or fireplace make sure to have it inspected once a year to make sure it is not releasing deadly carbon monoxide fumes. However, you don’t want to get your air ducts cleaned just to have them cleaned.
Look for the following signs to tell if your ducts need to be cleaned:
- Visible mold on the ducts or other heating and cooling components
- Vermin in the ductwork
- Dust, debris, and other particles clogging the ducts and being released through supply registers
If you decide your ducts need to be cleaned here are some tips to ensure you deal with a reputable company that cares about your situation and your well-being:
- Only deal with a reputable and professional company. Make sure you check for licensing, look up reviews online, and ask for references
- Make sure you let the cleaning company know they can’t use biocides or chemical treatments because of your COPD
- Ensure the company will protect you and whoever else lives in your house from being exposed to chemicals and contaminants that may come loose during the cleaning
- Leave your house while they clean your ducts
Get Rid of Chemically Based Cleaning Supplies

No matter how good of a job they do, chemically based cleaning supplies can be detrimental to your COPD symptoms and spark an exacerbation whether you’re doing the cleaning or not. However, there is more risk involved if you are the one cleaning.
The mix of chemicals in each cleaner gives off fumes that you are breathing in every second you clean and for minutes, or in some cases, hours after you finish. There may be a few items you can’t do without like plain bleach or ammonia, but it would benefit you to remove as many chemically based cleaners from your house as possible. Look for “green” cleaners that are all natural or you can use a water and vinegar solution and baking soda. There aren’t many things vinegar and baking soda can’t clean.
We recommend using vinegar and baking soda since neither of them are lung irritants. Here are some “recipes” and instructions for cleaning solutions using vinegar, water, baking soda, dish detergent, and ammonia (when needed).
Remember, when using ammonia or bleach to clean you will want to keep the mixture away from your face so you don’t breathe in the fumes. If possible, we recommend using a mask or respirator when using ammonia or bleach.
Toilet Cleaner
- Pour two cups of baking soda around the inside of your toilet bowl and scrub with a long handled brush to prevent bending at your waist and then flush the toilet when you finish scrubbing
- Pour two cups of vinegar inside the toilet bowl and swish around the entire bowl and then flush the toilet
- Make sure your toilet is not clogged when using this method to clean. If it is clogged the baking soda and vinegar will react and that’s a mess no one wants to deal with
Carpet Cleaner/Deodorizer
- Sprinkle baking soda over the affected area
- Let the baking soda sit and do its work (the longer it sits, the better job it does) and it’s okay if you walk on the area you are treating
- After you let it sit you will vacuum the treated area thoroughly
All-Purpose Cleaner
- Get a large spray bottle and put a half cup of baking soda into the bottle
- Fill with enough water to dissolve the baking soda
- Very slowly add a cup of vinegar to the bottle (the solution will begin to fizz a lot which is why you add the vinegar slowly)
- Top the mixture off with water and let it sit overnight
- In the morning flip it end over end to mix the solution (there will be more fizzing)
- When the fizzing stops your solution is ready to use
Grease Cutting Cleaner
- Follow the same recipe above for the All-Purpose Cleaner, but add a teaspoon of dish detergent
Window Cleaner
- Mix warm water with one cup of vinegar and two capfuls of ammonia
- Wear a mask or respirator and mix away from your face
- Wear mask or respirator as you clean with the solution
Tips to Clean Effectively and Efficiently with COPD
Before you start cleaning there are some tips and techniques you can use to conserve energy, cut out uncomfortable movements, and protect yourself from inhaling dust, fumes, and other particles while cleaning in a more effective and efficient way. Always remember, take frequent breaks as often as you need them while cleaning.
Tips to Remember While Vacuuming

When it comes to vacuuming it’s all about synchronizing your breathing pattern with the physical act of pushing/pulling the vacuum. Ideally you will want to use the pursed lip breathing technique.
- Take a deep breath before you start the vacuum
- Synchronize your breathing pattern with your movements as you push and pull the vacuum
- Exhale as you push the vacuum
- Inhale as you pull the vacuum
- Good posture is key and will keep your diaphragm open making it easier for you to breathe
- When emptying the vacuum, use a damp newspaper to trap dust particles and reduce the amount of dust particles getting in the air
Tips to Remember While Dusting
Dusting is very intimidating to some COPD patients and that’s understandable. It may seem like you are playing with fire by stirring up a known lung irritant, however these tips will reduce your exposure to dust particles and help you conserve energy along the way.
- Use a mask to prevent yourself from breathing in loose dust particles, we recommend a respirator just to be safe
- If possible dust while sitting down, this will eliminate the need for you to bend over to dust and it will conserve energy for later in the day
- When dusting areas that are hard to reach, use a long-handled duster to avoid reaching or climbing
- Avoid excessive furniture so you don’t have to move items around just to clean
Tips to Remember While Cleaning Your Floors

Cleaning your hard surfaced floors is very similar to vacuuming. You will want to focus on your pursed lip breathing technique and synchronize your breathing pattern with the physical act of pushing/pulling your broom or mop. If possible, avoid kneeling and scrubbing because it requires a lot of energy and bending over which can make it harder for you to breathe.
Sweeping/Mopping Your Floors
- Stand tall with good posture to avoid bending at your waist
- Synchronize your breathing pattern with your movements as you push and pull the mop/broom
- Inhale as you push the mop/broom
- Exhale as you pull the mop/broom
- Use a long handled dust pan when sweeping
- When possible use floor coverings that are low maintenance
Wiping Spills and Picking Up
- Use a small mop to wipe up spills to prevent bending at your waist or kneeling and scrubbing
- Use pick up tongs to pick articles up from the floor
- Use paper towels to reduce your laundry load
Kneeling and Scrubbing Your Floors
As stated above, if possible you should avoid kneeling and scrubbing your floors. However, if you absolutely have to here are some tips on how to scrub your floors with COPD:
- Use the pursed lip breathing technique
- Start in the kneeling position
- Take a deep inhale before bending down to scrub
- As you exhale bend down to start scrubbing
- Take as many breaks as you need
Tips to Remember While Making Your Bed
The first chore almost any of us had to do was make our bed. Now that you have COPD that chore takes a lot more time and a considerable amount of energy to complete. It’s easiest to make your bed if you do it bit by bit and don’t try to rush. Here are some helpful tips to use:
- Use the pursed lip breathing technique
- When straightening sheets do one side at a time
- Unfold your linen
- Line it up with the center of your bed
- Complete the side you are working on
- Move on to the other side
- When putting new sheets on do one side at a time
- Put bottom sheet, top sheet, and your blanket on all at once
- Tuck the bottom sheet on one side
- Tuck the bottom sheet on the other side
- Put pillows in your pillow case
Remember, don’t over exert yourself while cleaning. Take as many breaks as you need and enlist help from family and friends when possible. It might seem like a daunting task, but if you clean in bits and pieces rather than all at once you will be able to accomplish more without over exerting yourself.
Click Here to Go Back To The Top7. A Fingertip Pulse Oximeter is a Necessity
A fingertip pulse oximeter can vastly improve your chances of detecting early signs of an exacerbation and in turn it can help you prevent them from happening. So whether you were diagnosed with stage one COPD or stage four COPD, you should absolutely own a pulse oximeter.
Fingertip pulse oximeters work by using an infrared beam that reads your blood oxygen levels and your heart rate in a matter of seconds. Once it calculates your blood oxygen levels and your heart rate it will display the numbers on an easy-to-read screen. How can these readings be used to detect warning signs of an exacerbation? How can you use them to prevent exacerbations in the future?
As you regularly use a pulse oximeter you will notice a pattern in your blood oxygen levels that correlates with your activity level. When you are more active your oxygen levels may dip below normal for a little bit, which is expected since you were exerting yourself. When you are resting you will notice your oxygen levels don’t change much. This is where the regular use of a pulse oximeter will come in handy.
Throughout the day you will want to use your pulse oximeter to check and record your blood oxygen levels. This will help you learn what your normal blood oxygen levels are after exertion and at rest. As stated above, it is common for your blood oxygen levels to dip below normal after exertion, but they should steadily climb back up to your normal range. However, it’s a major red flag if your blood oxygen levels start to dip below normal when you are at rest.
A study done by R.W. Vandivier, from the Department of Medicine, Division of Pulmonary Sciences and Critical Care Medicine, at the University of Colorado at Denver concluded that the biggest red flag indicator of a COPD exacerbation is when your blood oxygen levels dip below 90% at rest. The other major indicators were; shortness of breath, FEV1, and coughing.
To help you get in the habit of using your pulse oximeter and recording your readings, here are some general times of when you should test your blood oxygen levels:
- Right when you wake up and get out of bed
- After you complete a chore or physical activity
- When you feel short of breath
- When you are sick
- When you are at high altitudes
- Before you go to bed
Aside from those times listed above, you should regularly check your blood oxygen levels throughout the day. A good time frame is once every two hours. This will help you get in tune with your body and you will begin to recognize how you feel when your blood oxygen readings are at a certain level.
If at any point your blood oxygen levels dip below 90% at rest, you should contact your doctor and seek medical attention immediately as this may be a sign you are experiencing or are about to experience a COPD exacerbation.
Click Here to Go Back To The Top8. Create a COPD Action Plan with your Physician
Having a COPD action plan can mean the difference between noticing and managing your exacerbation early enough to avoid hospitalization and getting hospitalized from your exacerbation. How might you ask? Well a COPD action plan is a plan created by you and your doctor to help you decide what action to take when you notice signs of an exacerbation.
Much like asthma action plans, COPD action plans have proven to be effective and follow the same three zone formula. The first zone is the green zone. The green zone means you are doing well and able to perform normal routines.
Next is the yellow zone. The yellow zone means you are having a bad day or are experiencing a flare-up.
The last and final zone is the red zone. The red zone is extremely dangerous and means you need to call 911 to get medical attention immediately. We will go more in-depth on the different zones shortly.
Before we go more in-depth on how the COPD action plan works, it’s important for us to tell you that this mock-up action plan is just a general action plan. You will have to sit down with your doctor and custom tailor your COPD action plan to your individual needs and current medical situation.
Green Zone
If you are in the green zone, you are good to go about your daily routines like normal. You aren’t coughing more than normal, you aren’t producing more phlegm, and you don’t have a constant feeling of breathlessness.
Actions to Take in the Green Zone
- Take your medications exactly as prescribed by your doctor
- Use your oxygen exactly as prescribed by your doctor (if prescribed oxygen)
- Continue your regular diet and exercise program
- Continue to avoid COPD triggers like cigarette smoke and chemically based cleaners, etc.
When you are in the green zone you don’t have many actions to take because you are already feeling well. It’s imperative that you continue taking your medication as prescribed by your doctor and that you use your supplemental oxygen as prescribed. By doing all of this you are giving yourself the best opportunity to successfully manage your COPD and prevent exacerbations from occurring.
Yellow Zone
If you are in the yellow zone you are either having a bad day or are experiencing a flare-up of symptoms. You may be feeling more breathless than normal, have less energy or feel more tired than usual, increased phlegm production (may notice a change in color), and you may have swelling of the ankles or feet. On top of those symptoms you may be taking your quick relief medications more often than normal, but it doesn’t help alleviate your symptoms.
Actions to Take in the Yellow Zone
- Continue to take your medications exactly as prescribed by your doctor
- Use quick relief medication every X hours
- The number of hours will be determined by you and your doctor when you create your action plan
- Begin use of corticosteroids as prescribed by your doctor
- Your doctor may prescribe this for you to have on hand in case of an emergency
- Start oral dose of antibiotics
- Your doctor may have prescribed this for you to have on hand
- Use your oxygen all-day and all-night, as prescribed by your doctor
- You may have to increase your flow rate, but that is determined by your doctor when you create the action plan
- Get plenty of rest
- Pay close attention to your diet
- Certain foods may make it harder to breathe
- Avoid soda and alcohol
- They are known to make it harder for you to breathe
- Use pursed lip breathing to make it easier for you to expel air from your lungs
- Use proper coughing techniques to help you get rid of phlegm
- Avoid cigarette smoke and all lung irritants at all costs
- Steer clear of anyone who may be sick
- If symptoms don’t improve, call for help immediately
The yellow zone can be very stressful and scary and when you become more stressed it can worsen your symptoms. Do your best to relax and take it slowly. Your main focus will be managing and alleviating your symptoms to the best of your ability within the action plan.
Red Zone
If you are in the red zone it means you are having a really bad day and are experiencing a COPD exacerbation. You may be unable to breathe unless you are sitting up in a chair with your AC on. It may be extremely difficult to move without getting short of breath. You may have a fever or the chills along with confusion or drowsiness. You may even be experiencing chest pains. If you feel like you are in the red zone you need to take immediate action.
Actions to Take in the Red Zone
- Take immediate action and call 911
- Do not call your doctor, you need immediate attention
- Do not have someone drive you to the hospital, it will take you too much time
- Call 911 to have paramedics come and give you immediate medical attention
The red zone is exceedingly scary and it’s even life threatening. It’s a necessity to take immediate action to get you the medical attention you need.
Remember, the COPD action plan above is a general outline and may not work for you. Call your doctor to set up an appointment to create your very own COPD action plan.
Once you create your COPD action plan you can use this checklist provided by COPD.com to help you stay up-to-date with your COPD symptoms and general health for your next doctors visit.
Click Here to Go Back To The Top9. Stay on Top of Medications and Vaccines

By effectively treating and managing your symptoms you should be able to manage and prevent COPD exacerbations, for the most part. This isn’t saying that by managing your symptoms you won’t ever experience an exacerbation, but it will help minimize the amount of exacerbations you experience and that is the ultimate goal. It goes without saying, but there is a method to your doctor’s madness. What he or she prescribes serves a purpose and it’s important to remember that as you continue your constant battle with COPD.
In order to efficiently and effectively manage your COPD you absolutely must take your medications exactly as prescribed by your doctor. As stated above, the goal of treating COPD is immediately treating and managing symptoms, so your doctor may change your medication or dosage depending on how you respond.
Since everyone responds differently to certain types of medication, we aren’t going into detail on the different types of medications. However, we are going to cover COPD medication guidelines and best practices to help you stay on top of your medications to better manage your COPD.
COPD Medication Guidelines
- Take your medications exactly as prescribed by your doctor
- Even if you feel good, do not stop taking your medication unless you talk to your doctor first
- Take your medications at the same time every day
- Set a reminder on your cell phone or tablet to help you remember
- Have a routine for taking your meds
- Use a calendar and a pill box to help you stay organized
- Wash your hands before preparing or taking your meds
- Regularly refill your prescriptions two or three business days before your medications run out
- DO NOT wait until you are out of meds before you attempt to refill them
- If for some reason you forget to take a dose, take it as soon as you remember unless it is almost time for your next dose. Then simply skip your missed dose and resume your regular medication schedule
- DO NOT double up on your dosage to make up for the missed dose unless you are instructed to do so by your doctor
- DO NOT cut back on your medication dosage, you must take the full amount to get the full benefits
- DO NOT stop taking your medications for any reason without talking to your doctor first
- If you are concerned with how the medication is working or how it makes you feel ALWAYS consult your doctor before making any changes to your medication schedule
- Store your medications following the instructions on the bottle
- Frequently check to make sure your liquid medications haven’t changed color or formed crystals
- If they have changed color or formed crystals, throw them out and get new ones
- DO NOT take any OTC medicine or herbal remedies without speaking to your doctor first
- They could have adverse reactions with medications you are on now
Get Vaccinated for Your Own Good
There are several different benefits you will get from staying vaccinated with COPD. For starters, dealing with COPD on its own is tough enough, but when you add an illness like influenza or pneumonia to the mix it can be nearly impossible to manage. That’s one of the main reasons it’s so important to avoid big crowds during flu season and sick people in general. To keep yourself as protected as possible you will want to get these three vaccines unless your doctor recommends against it.
Flu Vaccine
The flu is an extremely dangerous illness for COPD patients to come down with. It can increase mucus production which will cause you to cough more, make you feel short of breath, and it can cause you to have a fever or the chills just to name a few dangerous symptoms. Another danger of the flu for people with COPD is that it is notorious for turning into something more serious like pneumonia.
The benefits of a flu shot for people with COPD greatly outweigh the reasons you might avoid getting the vaccine. By getting vaccinated you will greatly reduce your chances of falling ill with the flu which also reduces your chances of the flu turning into pneumonia. On top of that, the flu vaccine may lower your chances of having an exacerbation.
Pneumonia Vaccine
COPD and pneumonia have a high comorbidity rate which means people with COPD are more likely to get pneumonia. Coming down with pneumonia can easily lead to experiencing an exacerbation or end you up in the hospital. By getting the pneumonia vaccine you will greatly reduce your risk of coming down with pneumonia. For the most part you will only need to get one pneumonia vaccine shot, however, your doctor may recommend a second shot.
Pertussis Vaccine
While the pertussis vaccine isn’t as important as the flu or pneumonia vaccines, it still has its benefits for people with COPD. Pertussis is known as whooping cough and it can cause some major problems if you come down with it.
It may start as a normal cold with symptoms ranging from a mild cough to a low fever. However, after a week your mild cough will turn into long coughing spells that end with a whooping sound as you try to get a breath in after your coughing spell. Combining your COPD with whooping cough can lead to COPD exacerbations. By getting the pertussis vaccine you will reduce your risk of coming down with it and it may help you control your COPD.
Always consult your doctor about getting vaccinated. He or she will recommend what is best for you.
Click Here to Go Back To The Top10. Dieting Makes A Huge Difference
Having a healthy and COPD friendly diet is more than just making healthy choices, it’s about making smart and strategic choices that will improve your quality of life. By eating the right foods and eliminating the bad stuff from your diet you can boost your immune system, improve your lung function, and in turn, reduce your chances of experiencing an exacerbation.
It’s important to remember that you need to talk to your doctor before making any major changes in your diet. They may recommend going a different route or advise against a certain type of food depending on your personal situation.
In this section we will go in-depth as to what to add and what to remove from your diet and why. We will also cover some tips to help you prepare and eat your meals without using all of your energy.
COPD Super Foods
When you are battling a disease like COPD, you want to give yourself every possible advantage to manage your symptoms. By adding the following COPD super foods to your diet you may boost your immune system, increase your energy levels, and improve your lung function.
Remember, before you make any changes to your daily diet you should consult your physician or nutritionist.
Omega-3 Fatty Acids

One of the most common symptoms of COPD is inflammation in your lungs. Although your doctors prescribe medicine to help alleviate inflammation in your lungs, you can add omega-3 fatty acids to your diet to help naturally fight off the inflammation. Along with reducing inflammation in your lungs, the long list of benefits you can get from omega-3 fatty acids includes; relieving joint stiffness and pain, help you manage depression, and added protection against Alzheimer’s and dementia to name a few.
To increase your consumption of omega-3 fatty acids, consider adding these foods to your grocery list:
- Fatty Fish
- Salmon
- Herring
- Sardines
- Lake Trout
- Tuna
- Anchovies
- Bluefish
- Mackerel
- Sturgeon
- Walnuts
- Butternuts
- Flaxseed
- Soybeans
- Flaxseed Oil
- Soybean Oil
- Canola Oil
Fresh, Bright, and Colorful Vegetables

Fresh veggies are an important part of any diet. However, it is the colorful and vibrant vegetables that have the most benefits for your COPD diet. Bright colorful veggies are packed to the brim with nutrients including; vitamins, minerals, antioxidants, and phytochemicals that help protect your body from free radicals that cause damage to your cells and tissues. Flash frozen vegetables are a good substitute if you are out of fresh veggies or don’t have the energy to prepare them. Here is a list of examples of vegetables for you to choose from:
- Broccoli
- Squash
- Sweet Potatoes
- Carrots
- Leafy Greens
- Brussel Sprouts
- Tomatoes
- Cucumbers
Whether you are just grabbing a snack or eating a full meal a good general guideline to follow is the “Half Plate Rule”. The Half Plate Rule is very simple and easy to follow, simply make your snack or meal and fill half of your plate with fruits or veggies. This will help ensure you are getting enough fruits and veggies in your diet.
Fresh, Bright, and Colorful Fruits

Just like the fresh veggies, incorporating fresh and brightly colored fruits into your diet is a necessity. Bright colored, fresh fruits are rich in antioxidants, vitamins, minerals, and phytochemicals which play an important role in protecting your lungs. In fact, a recent study has suggested that adding just one more serving size of fruit (100 grams) a day may lower your mortality risk by as much as 24%. Here is a list of fruits to choose from:
- Apples
- Bananas
- Oranges
- Watermelon
- Peaches
- Pears
- Berries
- Cherries
- Grapes
- Cantaloupe
When you are eating a snack or a full meal, remember to use the Half Plate Rule and fill up half of your plate with fruits and veggies. This will help ensure that you are getting enough fruits and veggies in your diet.
Fiber, Fiber, and More Fiber

Fiber has numerous benefits for your general health from regulating blood sugar levels to lowering your cholesterol. For COPD patients like yourself, fiber is important because it helps with digestion and can help control your weight. By maintaining a healthy weight you are lowering your risk of experiencing an exacerbation and boosting your energy levels. As a rule of thumb, women are recommended to consume 21-25 grams of fiber every day while men are recommended to consume 30-38 grams of fiber every day.
Here is a list of foods that are rich in fiber that you may want to consider adding to your diet:
- All-Bran Cereal
- Whole Grain Bread
- Brown Rice
- Oatmeal
- Fresh Fruit
- Fresh Vegetables
- Nuts
- Flaxseed
Remember to consult your doctor or nutritionist before changing your daily fiber intake. They may recommend a different amount to accommodate your needs.
Jumping for Soy

Although more research studies still need to be conducted, a research study done by Dr. Fumi Hirayama and Professor Andy Lee from Curtin University of Technology in Australia monitored 300 COPD patients and 340 non-COPD patients in the same age range to see how different levels of soy consumption affected the patients and the control group. The results of the study were promising. More soy consumed translated into fewer breathing problems, particularly the feeling of breathlessness and improved lung function. The group that saw the most benefits from soy consumed almost 60 grams per day. Here is a list of soy based foods to add to your diet:
- Tofu
- Natto
- Edamame
- Soy Milk
- Bean Sprouts
- Soy Nuts
Although more research is needed, the results were extremely promising. As long as your doctor or dietician approves, adding soy to your diet may improve your lung function and reduce your feeling of breathlessness.
Foods You Want in Your Diet
Along with the COPD super foods listed above, you will want to make sure you eat lean protein, whole grain foods, and overall nutritious foods. By incorporating these foods in your diet, you will provide your body with the calories and nutrients you need to sustain energy levels, boost your immune system, and repair muscles.
Lean Protein

Lean protein is an important aspect to almost any healthy diet, including your COPD diet. It is essential to repair muscles, it helps maintain muscle mass, it’s good for your heart, and it provides you with good “clean” energy. The reason why we emphasize lean protein is because lean proteins are lower in saturated fats and cholesterol. Here are some examples of lean protein:
- Fish High in Omega-3 Fatty Acids
- Chicken (particularly white meat)
- Beef (chuck shoulder, top sirloin, round steaks, roasts)
- Pork (pork loin, tenderloin, ham)
- Soy Foods
- Eggs
Whole Grains

As you already know, living with COPD requires a lot of energy. To satisfy your body’s need for energy, substituting simple carbs like white bread or white pasts for whole grain foods will not only help supply you with the energy you need, but whole grains have several different vitamins and minerals that will benefit your COPD.
Whole grain foods are complex carbohydrates that provide you with a healthy amount of calories, essential B vitamins, iron and magnesium. The calories and complex carbohydrates in whole grain foods are responsible for providing you with long-lasting energy to help you make it through the day.
Apart from providing long-lasting energy, whole grain foods are packed with nutrients that are beneficial for your COPD. Whole grain foods are high in B vitamins which are known to help improve your immune system which may have weakened due to your COPD. Whole grain foods are also high in fiber which helps with digestion and maintaining a healthy weight to lower your chances of exacerbating your symptoms. The magnesium in whole grain foods is necessary for protein production in your body and muscle contractions. Combine magnesium with calcium and the two act like a natural antihistamine. Finally, iron plays a vital role in treating and managing your COPD. It is a major component of hemoglobin which is responsible for carrying oxygen through your blood.
If you aren’t sure what counts as a whole grain food, here is a list of examples:
- Amaranth
- Barley
- Buckwheat
- Corn
- Oats
- Quinoa
- Rice (brown, black, purple, red)
- Rye
- Whole Wheat
- Wild Rice
- All-Bran Cereal
Due to the nutrients and caloric value of whole grain foods it’s recommended that you incorporate them into almost every meal, especially breakfast. Starting your day off with all-bran cereal, oatmeal, or whole wheat toast will help jumpstart your day and provide you with energy for the whole day.
Nutritious Foods
While dieting for your COPD has very specific guidelines to follow, overall you just want to focus on eating healthier. Make smart, educated decisions at the grocery store and at your favorite restaurants. Opt for grilled chicken instead of fried. Choose water over sugary, carbonated drinks. Substitute vegetables for French fries. In the end, you are only benefiting yourself by making the healthy choices. On that note, we will discuss foods to avoid with COPD.
Foods to Avoid with COPD
Just like there are super foods for COPD, there are also foods that can easily have a negative effect on your COPD symptoms and potentially cause you to experience an exacerbation. By reducing the amount of these foods that you consume you may leave yourself feeling better, with more energy, reduce your feeling of breathlessness, and better manage your symptoms.
Sodium

A diet that is high in sodium can cause some problems with your COPD. For one, sodium is linked to a couple of different things that can cause your symptoms to flare-up; fluid retention and shortness of breath. When your body retains fluids you begin to feel full and bloated which can make it harder for you to breathe and it can make it extremely uncomfortable for you to move around. And any time something is linked to causing shortness of breath, it’s a no brainer to avoid it when you suffer from COPD.
Reducing the amount of sodium you consume can be tricky because some of your favorite foods might be high in sodium or you may not be aware of how much sodium there is in a certain food. Here is a list of foods that are high in sodium that you should be regulated:
- Regular Canned Vegetables
- Frozen Meals/T.V. Dinners
- Processed Cheeses
- Soy Sauce
- Deli Meats
- Hot Dogs
- Salted Snacks (chips, pretzels, nuts)
- Food Preserved in Brine (pickles, olives, sauerkraut)
- Table Salt
It’s extremely important that you read the nutrition labels on everything you eat. As a rule of thumb, unless your doctor has requested you reduce the amount of sodium in your diet, you will want to avoid meals or snacks if they have 300mg of sodium or more per serving.
Remember to consult your doctor or nutritionist before you make any drastic changes to your diet in regard to sodium intake.
Deep Fried Food
Deep fried foods aren’t good for anyone. However, when you suffer from COPD, fried foods should be eliminated from your diet completely. Fried foods can cause discomfort with your COPD because they are known to cause bloating and gas. Bloating creates pressure that pushes up against your diaphragm which makes it difficult and uncomfortable to breathe. Deep fried foods are also really bad for your heart, so it’s an added plus to eliminate these foods from your diet.
Cruciferous Vegetables

Cruciferous vegetables are a double-edged sword with COPD. On one side you want to get your recommended daily fiber and vegetable servings. On the other side cruciferous vegetables are known to cause gas and bloating. While these vegetables are a source of protein and a great way to get your daily servings of vegetables, you will want to make sure you pay attention to how they affect you when you eat them. If they cause serious bloating and gas and make it harder for you to breathe, start limiting yourself to find a happy medium. If it seems like you cannot eat these vegetables without problems, cut them out of your diet completely and find different alternatives to replace their nutrition value. Here is a list of some cruciferous vegetables:
- Broccoli
- Brussel Sprouts
- Cabbage
- Cauliflower
- Collard Greens
- Horseradish
- Kale
- Radish
- Bok Choy
Carbonated and Caffeinated Beverages

When focusing on a healthy diet, it’s easy to overlook how certain drinks can negatively affect your COPD. Drinks like soda, coffee, and energy drinks should be avoided as much as possible. Although drinking these beverages might not lead to an exacerbation, they can cause discomfort, dehydration, and an energy crash.
Carbonated beverages are known to cause bloating which can put more pressure on your diaphragm, they can make it uncomfortable and harder for you to breathe. Along with bloating, energy drinks and soda can dehydrate you and cause you to have an energy crash later in the day. This isn’t to say you can’t enjoy a soda every now and then, but it is best to limit yourself to ensure you stay comfortable and hydrated.
Caffeinated beverages should also be limited in your diet for a few different reasons. For starters, caffeine may react with some of your medications in a negative way. Always make sure you consult your doctor to find out if it’s okay to mix caffeine with your meds. Along with reacting to your meds, caffeine may cause you to feel anxious or nervous if you drink too much. Although that doesn’t sound very harmful, feeling anxious or nervous when you have COPD may lead to you feeling short of breath.
Caffeine also has the well-known crash effect. It might give you a boost of energy right off the bat, but within a few hours you will experience a crash and feel fatigued. If you are one of those people that absolutely has to have coffee in the morning, make the switch to decaf to eliminate the mid-day crash and nervous jitters.
Alcohol

There are several different ways alcohol negatively affects your COPD, so avoiding alcohol with COPD should be a priority. As a depressant, alcohol slows down your respiratory system and decreases your lung function. It also makes it harder to clear excess mucus out of your lungs. Add all three of those elements together and it’s a recipe for disaster for COPD patients.
Although more research is needed to fully understand how alcohol effects the lungs, it’s a known fact that alcohol lowers your glutathione levels. Glutathione is an antioxidant that helps protect your lung cells from free radicals and prevent cellular damage. When your glutathione levels drop it can worsen your COPD symptoms and possibly lead to an exacerbation.
Mixing alcohol with medications is a big mistake. Whether the alcohol has a negative reaction with your medication or it makes your medication ineffective, the results can be devastating. If the alcohol renders your medication as ineffective, you essentially missed taking that dose of meds and won’t receive the benefits. On the flip side, if the alcohol has a negative reaction with your medications, it could lead to further complications or even death.
Foods That Cause Heartburn/Acid Reflux
When it comes to foods that cause heartburn and acid reflux everyone is different. Something that may cause heartburn for one person may not affect you at all. Keep that in mind as you read this section.
First off, suffering from COPD puts you at a higher risk of developing acid reflux. That’s why it is important to pay attention to certain foods that might give you acid reflux or heartburn (a side effect of acid reflux). The reason why you want to avoid foods that cause acid reflux is because it can cause your COPD symptoms to worsen. Here is a list of foods that may cause you to experience acid reflux:
- Citrus Fruits (oranges, grapefruits, lemons)
- Acidic Juices
- Chocolate
- Pizza
- Spicy Food
- Garlic
- Anything You Already Know That Gives You Heartburn
You don’t have to cut these foods out of your diet completely, but it’s recommended that you limit your intake to prevent acid reflux and heartburn.
To help you get a head start on your diet, we have created a healthy summertime treats cookbook. Just click the image below to download your cookbook.
Click Here to Go Back To The Top
11. Vitamin D

Vitamin D has numerous benefits and it plays a crucial role in your overall health. It is known to strengthen bones, protect your body from bacterial and viral infections. Vitamin D improves mental sharpness and is known to lower your blood pressure. However, what you may not know is that vitamin D may have the ability to help you manage your COPD. Although more research is needed to be conclusive there have been multiple studies in the United States that show vitamin D can help prevent and protect you from COPD exacerbations.
How can a vitamin help prevent COPD exacerbations? One way vitamin D works is by protecting your body from bacterial and viral infections. Both bacterial and viral infections are known to cause COPD symptoms to worsen and can potentially cause you to experience an exacerbation. If you don’t get enough vitamin D you are leaving your body unprotected from infections and raise your risk of experiencing an exacerbation. Another study which was published in the Lancet found that supplemental doses of vitamin D3 prevented moderate to severe COPD exacerbations in patients with vitamin D deficiency.
While the only way to know if you suffer from vitamin D deficiency is to get tested by your doctor, here are some symptoms you may experience if you aren’t getting enough vitamin D:
- Bone Pain
- Muscle Weakness
- Cognitive Impairment
- You aren’t as happy as normal or have the blues
Although these symptoms are vague, it's important to know the signs of vitamin D deficiency. If you think you might suffer from vitamin D deficiency contact your doctor immediately to get tested. Getting enough vitamin D is going to benefit your overall health and your COPD.
If you go get tested and you do have a vitamin D deficiency your doctor will help you determine the best course of action. There are a number of different ways to get more vitamin D from supplemental vitamins, to certain foods, and of course sunlight. Here is a list of ways you can get more vitamin D:
- Sunlight
- Ultraviolet Lamps/Bulbs
- Fatty Fish (Omega 3 Fatty Acids)
- Fortified Orange Juice
- Fortified Milk
- Fortified Cereal
- Egg Yolks
- Cod Liver Oil
- Supplements
As always, consult your doctor before blindly adding more vitamin D to your diet. He/she will recommend a specific amount of vitamin D to relieve your deficiency.
Click Here to Go Back To The Top12. Regular Exercise for the Win
Exercising for COPD might seem counterproductive, especially when you find yourself out of breath after a simple task. However, the benefits you can reap from regular exercise are undeniable and unmatched. From improving your overall health, to protecting you from exacerbations, exercising with COPD needs to be a part of your daily routine as long as it is permitted by your doctor.
When exercising for COPD it’s important to incorporate strength, cardiovascular, stretching, and breathing exercises into your routine. By incorporating all exercise types into your routine you are ensuring that you are getting a well-rounded workout and you are going to reap the most benefits. Having 4 separate exercise categories to incorporate into your routine may seem intimidating, but each exercise type serves a great purpose. We will be going over each exercise category, giving you examples of exercises in each category, and show you how they will benefit you.
Breathing Exercises
Breathing exercises are some of the most important exercises for COPD. Shortness of breath, anxiety, and stress are all common symptoms of COPD and can lead to an exacerbation if not treated properly. Combine the feeling of breathlessness and throw in anxiety or stress and it’s a recipe for disaster. By regularly practicing these breathing exercises and using them when you are feeling short of breath, you can improve your quality of life and your COPD symptoms.
You may have already learned about these breathing exercises in pulmonary rehab, which is great, but it doesn’t hurt to get a little review to refresh your memory.
Pursed Lip Breathing
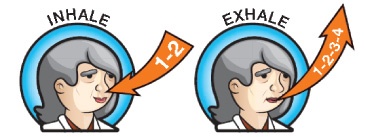
Pursed lip breathing is a proven technique that can help you regain your breath without your body having to work as hard. The damage to your lungs and airways caused by COPD can make it harder for you to expel all of the air from your lungs. If you don’t successfully get all of the air out of your lungs, the remaining air gets trapped which causes you to feel short of breath. The pursed lip breathing technique will cause you to use the correct breathing muscles to ensure you get as much air out of your lungs as possible. Here are step-by-step instructions on how to perform the pursed lip breathing technique:
- Inhale through your nose for two seconds (act like you’re smelling something)
- Pucker your lips like you are about to suck on a straw or blow out a candle
- Exhale slowly through your pursed lips, for at least 4 seconds or double the time you inhaled
- Repeat
This technique is perfect for the times when your shortness of breath seems like it won’t go away and it’s the ideal technique to use when you exercise. It’s important to get the timing and the technique down to ensure you are getting as much air out of your lungs as possible. If you need to, count in your head as you inhale and exhale to get as close to the recommended times as possible. You might be wondering, “How is pursed-lip breathing is so effective?” Here is a brief overview of how the pursed-lip breathing technique works:
- Slows down your breathing rate
- Keeps your airways open longer allowing you get rid of older, stale, and trapped air
- Increases the amount of time you can perform an activity or exercise
- Improves the exchange of oxygen and carbon dioxide in your body
- Makes it less work to breathe
Diaphragmatic Breathing
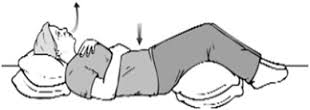
Compared to pursed-lip breathing, diaphragmatic breathing is more difficult to do without the help of a health professional. Before trying this on your own speak with your doctor or pulmonary rehab team to get properly trained.
The diaphragm is the primary muscle of breathing and it’s supposed to do most of the work. However, when you have COPD your diaphragm doesn’t work as well which leads to the muscles in your back, neck, and shoulders being used to help move air in and out of your lungs. The unfortunate part of this is that your back, neck, and shoulder muscles do very little to help move your air.
This is where diaphragmatic breathing can come into play.
The diaphragmatic breathing exercise essentially strengthens and re-trains your diaphragm to help expel as much air from your lungs as possible when you exhale. As you continue to practice this exercise your diaphragm will continue to regain strength and in turn help you breathe better. Here are the step-by-step instructions for diaphragmatic breathing:
- Sit back and relax or lay down flat on your back
- Place one hand on your chest
- Place your other hand on your stomach
- Inhale through your nose for approximately two seconds
- As you inhale you stomach should move outward farther than your chest
- Use pursed-lips as you exhale and gently press on your stomach
- Repeat
Cardiovascular Exercise
A cardiovascular exercise is any exercise that involves working large muscle groups in a rhythmic and consistent way that raises your heart rate. Cardiovascular exercises, AKA aerobic exercises, work wonders when you are trying to improve your COPD symptoms and prevent exacerbations by strengthening your lungs, improving your blood circulation, and reducing your stress, anxiety, and depression.
Out of the four different exercise categories, cardiovascular exercises are typically more intimidating when you have COPD which is understandable. However, once you get past the intimidation factor you will realize the great benefits these exercises have to offer. Here is a list of benefits you can see from doing regular cardio exercises:
- Strengthens your lungs
- Strengthens your heart
- Improves blood circulation
- Helps your body use oxygen more efficiently
- Improves your endurance
- Helps fight stress, anxiety, and depression
- Helps you sleep better
One really nice thing about cardiovascular exercises is that you can do them virtually anywhere. This is extremely beneficial for exercising with COPD because there are a number of different variables, like weather, that may prevent you from being able to do your normal workout. Even when the weather is too bad for you to go outside, you can still get your cardio workout finished at home. The list of cardiovascular exercises includes:
- Walking
- Jogging
- Water Aerobics
- Rowing
- Jumping Rope
- Skating
- Biking (indoor and stationary)
- Cross-Country Skiing
As you can see, there are some strenuous activities on that list, but you don’t just start there and hope for the best. It takes time to build up your endurance, strength, and confidence before you can tackle one of the harder challenges. If you don’t think some of those exercises are feasible, check out Russell Winwood. He is a COPD athlete who competes in marathons and other competitions around the country with stage 4 COPD.
When you first start with cardio exercises you will want to begin with walking as it is the least strenuous exercise. To gauge where you are at physically, walk as far as you can until you become short of breath. Once you become short of breath, stop to take a break and regain your breath. Then turn back and return home. As you continue to repeat this process you will build up your endurance and eventually will need to limit yourself based on time. As a rule of thumb, your workouts should be between 20 and 30 minutes as you don’t want to overexert yourself.
Remember to consult your doctor before adding cardiovascular exercises to your daily routine. He/she may have some specific recommendations or restrictions for you to follow as you build up your strength and endurance.
Strength Based Exercise
The saying goes “If you don’t use it, you lose it.” This is especially true when you suffer from COPD, if you don’t put your muscles to work your body deconditions and loses muscle mass. Allowing your body to decondition and lose muscle mass will cause you to feel short of breath more often than you used to. It will cause you to have less endurance and energy for the day, which makes it harder to complete your daily routines. This is where strength based exercise comes into the picture.
Upper Body

If your upper body begins to decondition and lose muscle mass you will have a harder time breathing and completing daily tasks. The feeling of breathlessness comes from air being trapped in your lungs no matter how hard you try and exhale. The muscles around your lungs help expel as much air from your lungs as possible when you exhale. As those muscles decondition your lungs will have a hard time getting all of the excess air out. The rest of your upper body muscles are responsible for helping you carry out daily tasks and routines, but their performance will suffer the longer they remain inactive. Your muscles will tire out much quicker which may cause you to become fatigued much earlier in the day than usual.
On the flip side, if you focus on strengthening your upper body you will reduce the feeling of breathlessness and you will have more endurance and energy to get you through the day. Here is a list of some upper body strength exercises that are linked to instructional videos on how to perform each exercise from Eldergym:
- Bicep Curls
- Side Shoulder Raises
- Upright Rows
- Overhead Elbow Extensions
- Overhead Press
- Elbow Side Extensions
Click on each exercise to see a proper example of how the exercise is done.
Before you add these workouts to your routine, speak with your doctor to ensure you are healthy enough to do them. It’s important to remember when you are using weights for training to use light weight dumbbells. Using light weight for strengthening your muscles can be just as effective as using heavy weights.
Lower Body

Just like your upper body, if you let your lower body decondition and lose muscle mass you will have noticeably less endurance and you will feel fatigue set in earlier in the day. As your lower body loses muscle mass and deconditions you will also notice your mobility start to decrease. If this vicious cycle were to continue, it would be detrimental to your overall health and cause your COPD symptoms to worsen.
By focusing on strengthening your lower body, you will not only combat the issues stated above, but you will soon see improvements in those areas. You will have more endurance throughout the day, you will have more mobility, and you will have seemingly more energy. As you remain active you will reap the benefits of improved circulation and oxygen usage, less time spent feeling breathless, and improved mental morale.
Although a lot of your cardio workouts can double as lower body strength workouts you will still want to make sure you incorporate some of these lower body workouts into your routine along with regular cardio workouts. Here is a list of some lower body strength exercises linked to instructional videos from Eldergym on how to perform each exercise:
- Squats
- Lunges
- Ankle Circles
- Hip Marching
- Knee Extension
- Calf Raises
- Sit to Stand
- Heel Stand
- Straight Leg Raise
- Hip Extension
Remember to speak with your doctor before adding a workout regimen to your daily routine. Always start off easy and work your way up in difficulty. The key is to not overexert yourself.
Stretching Exercises

Stretching is an important part of exercising that you need to incorporate into your workouts. It is the slow process of loosening and lengthening your muscles that is normally done before and after a workout. It is a proven method to help prevent injuries, soreness, and stiffness during and after your workout. Stretching not only improves your flexibility, but also your range of motion.
Before each workout it’s important that you stretch your muscles to improve blood circulation, loosen your muscles, and help prevent muscle strains and other injuries, especially the muscle group you are working out. If you are doing an upper body workout, it’s imperative that you focus on stretching your upper body muscles. If you are doing a lower body workout, you will focus on stretching your lower body muscles. However, you will still want to get a full body stretch in to ensure you are fully warmed up. Stretching after you work out is just as important as stretching before you work out. Stretching post workout will reduce muscle fatigue, reduce the feeling of soreness, and help prevent future injuries. Here is a list of some of the best stretches with linked videos from Eldergym:
Upper Body Stretches
- Shoulder and Upper Back Stretch
- Shoulder Rolls
- Neck Side Stretch
- Neck Rotation
- Shoulder Circles
- Shoulder Stretch
- Chest Stretch
- Overhead Reach
- Reach Back
- Triceps Stretch
- Hand Stretch
- Arm Raises
Lower Body Stretches
- Seated Lifts
- Standing Quadriceps Stretch
- Back Stretch
- Inner Thigh Stretch
- Calf Stretch
- Hip Side Stretch
- Hip Rotation Stretch
- Soleus Stretch
- Ankle Circles
- Hamstring Stretch
- Knee to Chest
- Ankle Stretch
Yoga

Yoga is a popular exercise that has recently been getting a lot of praise in the COPD community and for good reason. It is a low impact exercise that can be adjusted to any skill level and all the poses can be modified to your abilities. There have also been some different studies that have linked yoga to improved quality of life and improved lung function in COPD patients. In one study, 29 people with COPD followed a consistent 12 week yoga schedule and saw significant improvements in their lung function, quality of life, breathing ability, and inflammation in their lungs. Although the studies are recent and need more research to conclude the findings, the studies done on yoga and COPD are promising.
Through a series of poses, yoga uses strength, flexibility, and breathing to give you a meditative workout that benefits your mind and your body. The enhanced breathing techniques used in yoga can help you alleviate your feeling of breathlessness and improve your breathing ability. The meditation and relaxation techniques used can reduce your stress, anxiety and depression; all of which are commonly linked to COPD. Yoga will also strengthen your muscles across the board which will improve your breathing ability, your endurance, and your energy levels over time.
There are a few different ways you can practice yoga. You can do it at home with a DVD video or an online video, you can join a class at your local gym or rec center, and you can go to a yoga studio. No matter which method you choose, make sure you start light and work your way up in difficulty. You don’t want to overdo it. If you think yoga would be beneficial for you, speak with your doctor and look into enrolling in some classes to help you get started. It’s always easier to learn if you have hands on help.
Click Here to Go Back To The Top13. Get More Sleep

Adults are recommended to get anywhere between 6 and 8 hours of sleep every night. Getting enough sleep is essential to your overall health. When you suffer from COPD getting enough sleep is even more important. Sleep allows your body to repair itself, it’s good for your heart, your mood, and it helps you maintain a healthy weight. If you don’t get enough sleep with COPD it can cause your symptoms to worsen and weaken your immune system which can cause you to have an exacerbation.
It can be extremely difficult to fall asleep and stay asleep with COPD. There are many different reasons you might not be able to get quality sleep at night ranging from your sleep position to sleep apnea. Here is a list of the top reasons why you might have a hard time sleeping:
Medication
The type of medication and specified dosage might be interfering with your sleep schedule. If you are experiencing a difficult time falling asleep or staying asleep check your medications side effects to see if something you are taking is the reason for your problems. If you find something in your medications that might be causing this, DO NOT stop taking the medication. Schedule an appointment with your doctor to see if there is an alternative medication or if you can change your dosage to alleviate your sleep problems.
Sleep Position
Many COPD patients prop themselves up or sit up to sleep because breathing becomes more difficult when they lie down. However, sitting up or propping yourself up can make it difficult to stay asleep for a full 6 to 8 hours. If you find it uncomfortable and harder to breathe when you lie down to fall asleep, talk with your doctor about getting prescribed nighttime oxygen.Breathing Changes
When you fall asleep your breathing rate slows down and your respiratory system becomes less responsive. This isn’t normally a problem for healthy people, but when you suffer from COPD it can cause disruptions in your sleep cycle. If you notice yourself waking up in the middle of the night feeling short of breath talk to your doctor about getting prescribed nighttime oxygen and getting tested for sleep apnea.
Acid Reflux
Acid reflux is extremely common among COPD patients and it can cause some serious problems while you are trying to fall asleep and stay asleep. Acid reflux can cause heartburn, bloating, and stomach discomfort all of which can worsen your COPD symptoms and make it harder to breathe. If you suffer from acid reflux, speak with your doctor about treatment options that will not interfere with your medications.Mental Health
Anxiety, stress, and depression are all commonly linked to COPD for several different reasons. They can all cause you to have issues falling asleep and staying asleep by causing your mind wander aimlessly throughout the night. You can naturally fight anxiety, stress, and depression by having a healthy diet and exercising more and you can also speak with your doctor about getting a prescription to alleviate the symptoms.
Sleep Apnea
An estimated 10% to 15% of COPD patients suffer from sleep apnea. Sleep apnea is a disorder that occurs when your breathing is disrupted when you’re sleeping. The symptoms of sleep apnea include; loud snoring, frequent awakenings at night, daytime sleepiness, and morning headaches. If you experience these symptoms and have a hard time sleeping, contact your doctor to get tested for sleep apnea.
Despite these common reasons why you might have a hard time sleeping and staying asleep, there are several different ways you can combat them. Here are some tips that don’t require talking to your doctor:
- Your bed should be used for one of two actions; sleep or sex. Try not to watch TV, read, or simply lie awake in your bed because it will condition your mind to associate those activities with your bed and make it harder for you to fall asleep.
- If you cannot fall asleep within 20 minutes of lying down, get up out of your bed and do something calming and relaxing that will help you become sleepy and try again.
- Have a regular sleep schedule so you are waking up and falling asleep around the same time each day. This will help condition your mind and your body to know when it is time to go to sleep.
- If you drink caffeinated beverages, do not consume any caffeine within 5 hours of when you want to fall asleep.
- Try not to nap during the day to ensure you will be tired when it is time to go to sleep. If you must nap, set an alarm and keep your nap short.
- Get regular exercise to help tire your body and mind out before you go to sleep. However, avoid working out within 2 hours of when you want to go to sleep as this will make it harder to fall asleep.
- Make sure your bedroom is quiet, dark, and is at a temperature you find comfortable. Falling asleep when you are cold or hot can be extremely difficult, not to mention noise and light can keep you up all night.
- Don’t go to bed feeling hungry. Whether you finished eating dinner three hours ago or just recently, if you are still hungry grab a small protein filled snack to curb your hunger. Avoid sugary snacks and snacks that are high in carbohydrates as these food types will jump start your metabolism and keep you up longer.
If you still have a hard time sleeping after following these tips, get in touch with your doctor and see what options you have to take. Whatever you do, don’t just go out and buy over-the-counter sleep aids. Many over-the-counter sleep aids will slow your respiratory system down which is extremely dangerous when you suffer from COPD. Sleep aids can also have a negative affect when combined with some of your other COPD meds.
Time to Take Action
You just read 13 strategies to help prevent and manage COPD exacerbations…
Now it’s time for you to work these strategies into your daily routine.
Your first step is to pick a few of these strategies that seem manageable and make them a part of your daily routine. As you start to become more comfortable with these additions to your routine, pick a few more and start to work them in.
You will eventually get to a point where you have incorporated all of these strategies into your daily routine and you will have significantly reduced your chances of experiencing an exacerbation and you will be able to manage them much more effectively.
If you want to keep this post for future reference click the picture below to download a free copy of 13 Simple Strategies You Can Use Today to Help You Prevent and Manage COPD Exacerbations:
Related Blog Posts:
- COPD Awareness Month: The Ultimate Guide to Managing Your COPD in the Winter
- 59 Hacks and Tips You Can Use Immediately To Help Make Life With COPD More Manageable
- COPD Nutrition: Eating All of the Right Things
Sources:
http://www.copdfoundation.org/Learn-More/Pulmonary-Rehabilitation/Find-a-PR-Center-Near-You.aspx
http://www.mayoclinic.org/healthy-lifestyle/adult-health/in-depth/hand-washing/art-20046253
http://www.webmd.com/lung/copd/features/household-hazards-for-people-with-copd?page=3
http://blog.copdfoundation.org/clean-air-and-copd/
http://www.healthline.com/health/copd/managing-at-home#1
http://www.everydayhealth.com/copd/indoor-air-pollution-and-managing-copd.aspx
http://www.everydayhealth.com/copd-pictures/10-home-hazards-for-people-with-copd.aspx#01
http://www.everydayhealth.com/copd-pictures/common-copd-triggers-and-how-to-avoid-them.aspx#04
http://www.healthline.com/health/copd/humidity
http://www.diynatural.com/indoor-humidity-in-house/
http://www.everydayhealth.com/copd/weather-can-affect-copd.aspx
http://blog.copdfoundation.org/how-does-weather-affect-my-copd/
http://www.copdbfrg.org/?page_id=403
http://www.healthline.com/health/copd/allergies#3
http://www.pollen.com/allergy-weather-forecast.asp
http://www.physiciansweekly.com/reducing-exacerbations-in-copd/
http://www.ersj.org.uk/content/33/5/1031.full
http://www.healthcentral.com/copd/c/52325/170677/copd-action-plan/
http://www.copd.com/copd-care-plan/
http://www.webmd.com/chronic-obstructive-pulmonary-disease-copd-prevention
http://www.todaysdietitian.com/newarchives/td_020909p54.shtml
http://copd.about.com/od/copd/a/copddiet.htm
http://copd.about.com/od/copdandnutrition/tp/6-Copd-Super-Foods.htm
http://lunginstitute.com/blog/alcohol-worsen-copd/
http://wholegrainscouncil.org/whole-grains-101/whole-grains-a-to-z
http://lunginstitute.com/blog/foods-to-avoid-with-copd/
http://www.medscape.com/viewarticle/835873
https://www.vitamindcouncil.org/health-conditions/chronic-obstructive-pulmonary-disease/#
http://www.health.com/health/gallery/0,,20504538,00.html
http://www.copdfoundation.org/What-is-COPD/Living-with-COPD/Breathing-Techniques.aspx
http://www.everydayhealth.com/copd/breathing-techniques-for-copd.aspx
http://www.webmd.com/lung/copd/pulmonary-rehabilitation-for-copd
http://www.proactivecopd.com/patients-and-carers/exercises-for-copd-patients/strengthening-e/
http://blog.copdstore.com/the-ultimate-guide-to-mastering-your-copd-management-today#chapter8
http://www.proactivecopd.com/patients-and-carers/exercises-for-copd-patients/strengthening-e/
http://www.copdfoundation.org/What-is-COPD/Living-with-COPD/Exercise.aspx
http://lunginstitute.com/blog/how-can-yoga-help-copd/
http://eldergym.com/exercises.html
http://www.everydayhealth.com/copd/sleep-and-copd.aspx
https://lunginstitute.com/blog/7-things-you-need-to-know-about-sleep-and-copd/









