Need help? Call us:
- Questions? Call us toll-free +1-800-520-5726

CPAP Masks Finder
Discover your perfect mask fit
- Portable Oxygen
- Home Oxygen
- Oxygen Accessories
- CPAP Machines
- CPAP Supplies
- CPAP Masks
- Mobility
- Bathroom Safety
- Pediatrics
- New Arrivals
Summer Allergies in 2023: A Survival Guide for COPD and Respiratory Patients
Summer Allergies in 2023: A Survival Guide for COPD and Respiratory Patients

Springtime and Summer bring beautiful blooming flowers, pleasant weather, and the promise of new beginnings. However, for individuals with COPD (Chronic Obstructive Pulmonary Disease) and respiratory conditions, the arrival of spring also signifies the onset of seasonal allergies.

Allergens such as pollen, dust, and mold can trigger respiratory symptoms and exacerbate existing conditions. In this comprehensive guide, we will explore various survival tips and essential tools to help COPD and respiratory patients navigate this long and irritable allergy season in 2023.
As summer approaches, individuals with COPD (Chronic Obstructive Pulmonary Disease) and respiratory conditions face the challenge of dealing with seasonal allergies. The arrival of blooming flowers and pleasant weather also brings allergens like pollen, dust, and mold that can trigger respiratory symptoms and worsen existing conditions.
In this comprehensive survival guide, we will explore various survival tips and essential tools to help COPD and respiratory patients navigate allergy season in 2023.Understanding Summer Allergies and What They Bring

To effectively manage spring allergies, it is important to identify common allergens and understand their impact.
Identifying Common Allergens
Pollen, dust mites, mold spores, and pet dander are the primary culprits during this season. By knowing your specific triggers, you can take appropriate measures to minimize exposure. Check local pollen forecasts regularly to stay informed about the current allergen levels.

When pollen counts are high, keep windows closed and avoid outdoor activities during peak allergy hours (usually early morning and late afternoon). To create a safer indoor environment, consider using air purifiers and HVAC filters equipped with high-efficiency particulate air (HEPA) technology. These devices can effectively filter out allergens from the air, reducing respiratory symptoms.
Here are some common allergens
Pollen, dust mites, mold spores, and pet dander are common allergens during springtime. Understanding your specific triggers can help you take appropriate measures.
Managing Exposure to Allergens
Maintaining a Healthy Environment
Start at home where you spend more of the days and nights! Keeping your living space clean and free from allergens is essential. Regularly dust and clean surfaces using a damp cloth to prevent airborne particles from circulating.

Invest in a vacuum cleaner with a HEPA filter, which can effectively capture allergens from carpets, rugs, and upholstery. By vacuuming frequently, you can reduce the presence of allergens in your home, creating a healthier environment for respiratory patients.
Regularly check local pollen forecasts, keep windows closed during high pollen counts, and avoid outdoor activities during peak allergy hours (usually early morning and late afternoon).
Tools and Devices to Keep you Home Free of Allergens
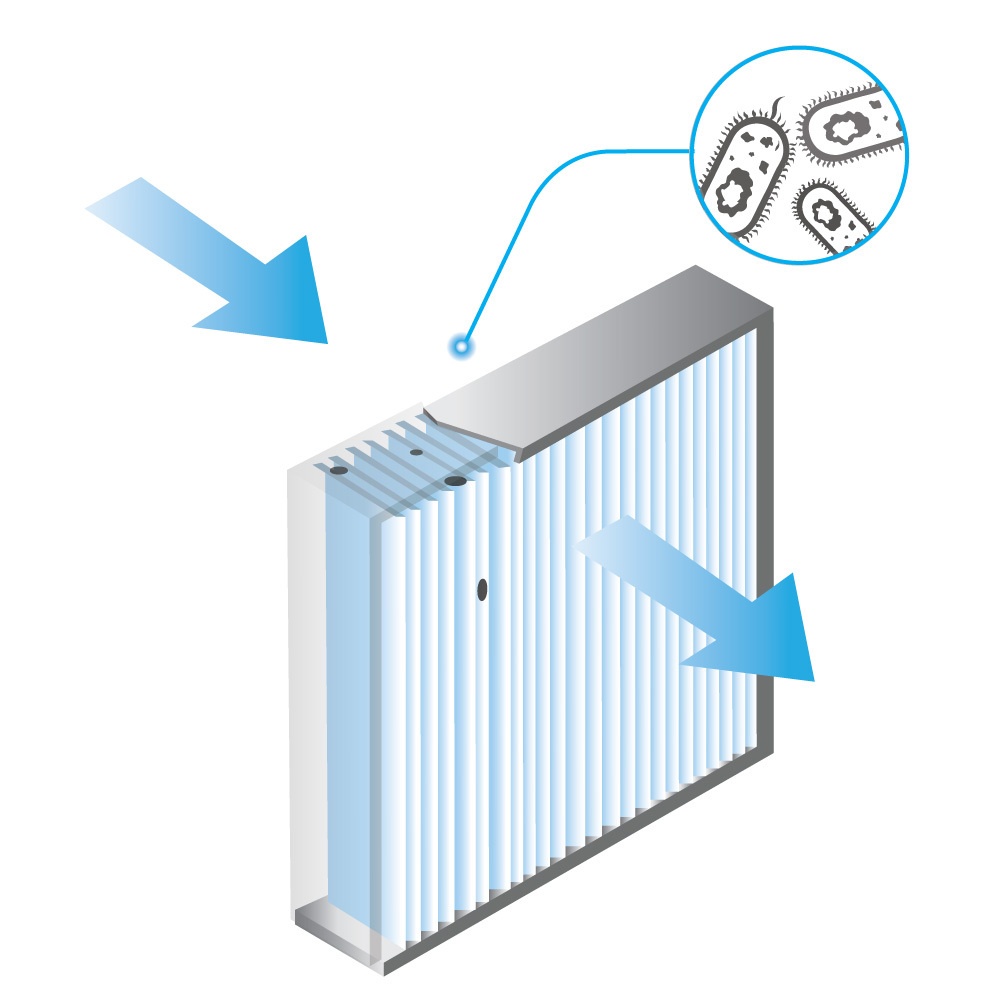
Air purifiers and HVAC filters with high-efficiency particulate air (HEPA) technology can help filter out allergens from indoor air, reducing respiratory symptoms.
Cleaning and Dusting

Regularly clean your living space, removing dust and allergens from surfaces. Use a damp cloth to minimize airborne particles while dusting.
Vacuuming: Consider investing in a vacuum cleaner with a HEPA filter to capture allergens effectively. Vacuum carpets, rugs, and upholstery frequently.
Tools and Devices: A high-quality HEPA vacuum cleaner can significantly reduce allergen levels in your home.
Monitoring Oxygen Levels

For COPD and respiratory patients, monitoring oxygen levels becomes crucial during allergy season, when symptoms can worsen. Portable oxygen concentrators provide a practical solution for maintaining a steady supply of oxygen while allowing patients the freedom to move around.
These lightweight and compact devices are ideal for outdoor activities and can significantly improve the quality of life for individuals with respiratory conditions.
Additionally, using a pulse oximeter a small, non-invasive device that measures oxygen saturation levels in the blood allows patients to monitor their oxygen levels at home and detect any potential issues promptly.
LPT Medical offers a range of reliable portable oxygen concentrators and high-quality portable oxygen concentrators to support COPD patients in managing their condition during allergy season.
Importance of Monitoring Symptoms and Treatment
COPD and respiratory patients should monitor their oxygen levels regularly, especially during allergy season when symptoms may worsen.
Portable Oxygen Concentrators: Portable oxygen concentrators provide COPD patients with the freedom to move around while ensuring a steady supply of supplemental oxygen. They are lightweight, compact, and ideal for outdoor activities.

Pulse Oximeter: A pulse oximeter is a small, non-invasive device that measures oxygen saturation levels in the blood. It can be used at home to monitor oxygen levels and detect any potential issues promptly.
Knowing When to Seeking Medical Support

If you experience severe allergy symptoms or notice a decline in respiratory function, consult your healthcare provider for a thorough evaluation and treatment options.
COPD exacerbations can occur when respiratory symptoms worsen suddenly, leading to a decline in lung function. It is important for COPD and respiratory patients to recognize the signs of an exacerbation and seek medical attention promptly.
While allergies can exacerbate respiratory symptoms, a COPD exacerbation may be a more serious condition that requires immediate medical intervention.

Experiencing a COPD exacerbation can be a distressing and frightening experience. Symptoms may include increased shortness of breath, wheezing, coughing (with or without mucus production), chest tightness, and fatigue.
Some individuals may also experience rapid breathing, bluish lips or fingertips, confusion, or a feeling of suffocation. The severity of symptoms can vary, but any significant increase in respiratory distress should not be ignored.
When COPD and respiratory patients seek medical attention during an exacerbation, they can expect a comprehensive evaluation and treatment plan tailored to their specific needs. The healthcare provider will conduct a thorough examination, which may include assessing lung function through spirometry or other breathing tests.
They may also inquire about the patient’s medical history, including any recent exposure to allergens or changes in medication.
Treatment for a COPD exacerbation may involve a combination of interventions, such as:
1. Oxygen Therapy: Oxygen may be administered through nasal prongs, a mask, or a portable oxygen concentrator, depending on the severity of the exacerbation. This helps increase oxygen levels in the blood and alleviate shortness of breath.
2. Bronchodilators: These medications help relax the airway muscles, allowing for improved airflow and easier breathing. They may be delivered through inhalers or nebulizers.
3. Steroids: Inhaled or oral corticosteroids may be prescribed to reduce inflammation in the airways, helping to relieve symptoms.
4. Antibiotics: If there is evidence of a respiratory infection, such as increased mucus production or fever, antibiotics may be prescribed to treat the infection and prevent further complications.
5. Pulmonary Rehabilitation: In some cases, healthcare providers may recommend pulmonary rehabilitation programs. These programs involve exercises, education, and support to help patients manage their respiratory condition and improve their overall lung function.
It is important to note that each patient’s treatment plan may vary based on their specific condition and the severity of the exacerbation. Healthcare providers will work closely with patients to develop a personalized plan that addresses their individual needs and goals.
In some instances, severe exacerbations may require hospitalization. This is typically reserved for cases where symptoms are severe and unresponsive to initial treatments, or when there are complications that need closer monitoring and intervention.
In the hospital setting, patients may receive additional treatments such as intravenous medications, supplemental oxygen, and close monitoring by a specialized medical team.
Healthy Diet
A well-balanced diet can boost your immune system and help reduce inflammation. Include fruits, vegetables, lean proteins, and omega-3 fatty acids in your meals.
Hydration: Stay well-hydrated to thin mucus secretions and keep airways moist. Aim for at least eight glasses of water per day.

Self-Care and Lifestyle Adjustments
In addition to medical interventions, self-care and lifestyle adjustments play a crucial role in managing summer allergies for COPD and respiratory patients. Adopting a healthy diet that includes fruits, vegetables, lean proteins, and omega-3 fatty acids can strengthen the immune system and reduce inflammation.
Staying hydrated is also essential, as it helps thin mucus secretions and keeps airways moist. Aim to drink at least eight glasses of water per day. Keeping a water bottle or a hydration tracker nearby can serve as a reminder to drink water regularly and maintain proper hydration levels.Conclusion
Summer allergies can pose challenges for individuals with COPD and respiratory conditions, but by understanding the allergens, maintaining a clean environment, monitoring oxygen levels with portable oxygen concentrators and pulse oximeters from LPT Medical, and seeking medical attention when needed, COPD and respiratory patients can navigate allergy season more effectively.
Recognizing the signs of a COPD exacerbation and promptly seeking medical attention is crucial for managing the condition and preventing further complications. COPD exacerbations can be distressing, but with comprehensive evaluation and personalized treatment plans, healthcare providers can help patients alleviate symptoms and improve lung function.
Remember, each patient’s experience may vary, and treatment plans will be tailored to individual needs. By working closely with healthcare providers, COPD and respiratory patients can receive the necessary support, including oxygen therapy, bronchodilators, steroids, and antibiotics, as well as access to pulmonary rehabilitation programs when appropriate.
By following the survival tips outlined in this guide, including understanding allergens, maintaining a healthy environment, monitoring oxygen levels, and seeking medical support when needed, COPD and respiratory patients can better manage spring allergies and maintain their respiratory health during this season.
Remember, you are not alone in this journey. LPT Medical provides a range of reliable tools and devices such as portable oxygen concentrators and oxygen accessories to support COPD and respiratory patients in effectively managing their condition. By taking proactive steps and utilizing the right tools, you can navigate allergy season with greater confidence and improve your overall quality of life!
































































Comments are closed