Need help? Call us:
- Questions? Call us toll-free +1-800-520-5726

CPAP Masks Finder
Discover your perfect mask fit
- Portable Oxygen
- Home Oxygen
- Oxygen Accessories
- CPAP Machines
- CPAP Supplies
- CPAP Masks
- Mobility
- Bathroom Safety
- Pediatrics
- New Arrivals
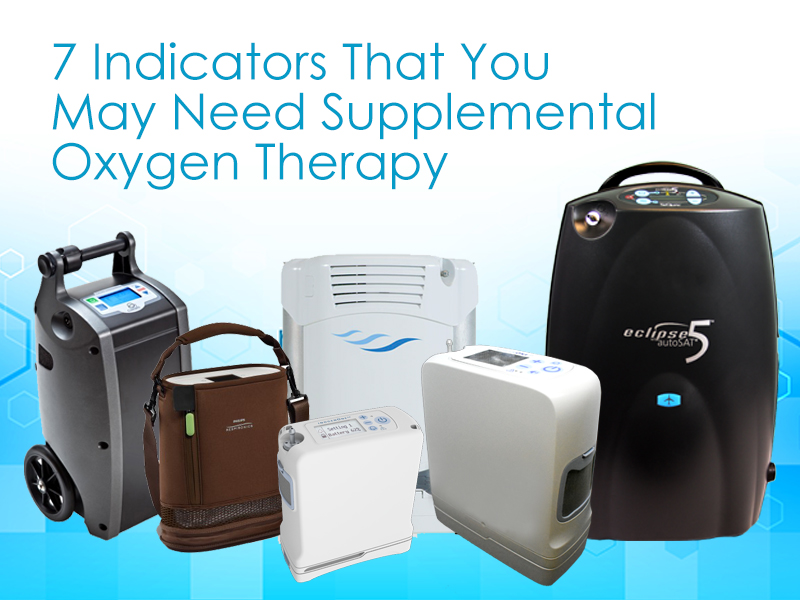
7 Indicators that You May Need Supplemental Oxygen
7 Indicators that You May Need Supplemental Oxygen
There is a lot that can be done through medicine and lifestyle changes to allow those battling a respiratory disease to live a full and independent life. Even those who require supplemental oxygen are free to travel with portable oxygen concentrators. Supplemental oxygen technology is advancing further all the time. Concentrators are getting more advanced, smaller, lighter, and more powerful all the time.
Oxygen deprivation is one of the most dangerous aspects of respiratory disease. When managing a serious lung condition it is important to monitor your symptoms closely. Lung disease progresses when symptoms escalate quickly, commonly referred to as symptom exacerbation.
Blood oxygen, or saturation levels, is the measurement of how much oxygen is contained in your bloodstream. Oxygen is carried by your blood to every cell and organ in your body through your bloodstream.
As a lung condition progresses, those who are battling a lung condition sometimes require supplemental oxygen in order to maintain oxygen saturation above 90%.
Low Blood Oxygen Saturation can Cause a Variety of Issues
- Shortness of Breath
- Chest Pain
- Confusion
- Balance or Coordination Issues
- Rapid Breathing
- Headache
- Dizziness
If you have any of these symptoms or even suspect that your oxygen levels are low, don’t hesitate to reach out to a medical professional.
The Seven Main Indicators That You May Need Oxygen
#1: You Feel Short of Breath When Walking
It’s normal to feel short of breath when walking uphill or walking quickly over a long distance but, if you feel so short of breath while walking at a normal pace that you have to stop and take a break, that’s a telltale sign your oxygen levels are too low.
While being active it is important to be mindful of your breathing to ensure that you’re not holding your breath and that you are taking slow, even, deep breaths. Sometimes when we are about to tax ourselves physically, it can be a natural inclination to hold your breath to brace yourself. Doing this repeatedly will likely cause you to feel out of breath.
If you are experiencing anxiety, your body will increase your heart rate and cause your breathing to become quicker and shallower. This is a natural fight or flight response. If you are feeling short of breath, try to keep your emotions in check. Remain calm, begin doing some pursed lip breathing or diaphragmatic breathing and see if normal breathing resumes. If not, use your rescue inhaler or take whatever measures that your doctor or respiratory therapist has instructed you to do in these situations.
#2: Your Heart Races When You Walk At a Slow or Moderate pace
Again, rapid heart rate can stem from anxiety. However, if you’re not feeling anxious, it could signal a heart or lung condition.
When your brain senses there’s not enough oxygen, it sends the heart a signal to beat faster to circulate more oxygen, so your heart rate goes up. This is also part of your body’s fight or flight response.
If you keep walking, you may feel dizzy or experience heart palpitations. You may even start to sweat, since your body will react like you’re exerting yourself and try to pump blood quicker in its attempt to circulate more oxygen. This is a signal from your body that you need to seek the advice of your doctor about supplemental oxygen therapy.
#3: Your Walking Oxygen Blood Saturation Is Below 88%
If you’re experiencing shortness of breath or any of the other symptoms of hypoxia that we’ve discussed, and if your COPD is more advanced, your pulmonologist will likely order a six-minute walk test. The doctor will put a pulse oximeter on your finger and observe you while you walk on a treadmill or up and down the hallway in the office.
When we’re sitting still, we don’t need as much oxygen, but the moment we get up and start walking, our bodies require more oxygen to provide energy and to allow muscles to function.
Your pulmonologist will likely discuss what your personal normal oxygen saturation level is. Those with normal lung function usually have oxygen saturation numbers in the upper 90 percentile. Levels above 90% are generally considered normal but if you consistently have saturation levels below 88%, your doctor or pulmonary specialist will likely prescribe supplemental oxygen. They’ll let you know what range of saturation you should maintain, and when you should seek medical attention. Be sure to monitor your levels carefully.
#4: You Feel Tired During the Day
Everyone feels tired sometimes but people with COPD or other respiratory conditions are more likely to have trouble sleeping. Symptoms like coughing and wheezing can definitely disrupt your sleep, but low oxygen levels overnight can also impact sleep quality and leave you feeling tired during the day.
If you wake up feeling confused and a little bit out of sorts, or have a slight headache, it may be because your oxygen levels are dipping to dangerously low levels as you sleep.
Everyone’s oxygen levels decrease a bit overnight, because breathing slows down. But, for someone with COPD, they may drop too low. In this case, your doctor may prescribe oxygen therapy for use overnight to help you get better rest.
First, your doctor will have to determine why your oxygen levels are dropping. Sometimes a condition such as congestive heart failure can cause your oxygen levels to drop when you’re in a horizontal position.
You may also have a sleep condition such as sleep apnea which may be affecting your oxygen levels as well as robbing you of restful sleep. Your doctor will probably want you to participate in a sleep study.
Sometimes you will have to go to a sleep center and get hooked up to monitors while you sleep so that they can see how often and to what extent your breathing is impared during the night. They also sometimes have machines that you can pick up and use at home that will record the same information. You will then return the equipment to the sleep center after your period of observation is over.
Once your results are analyzed your doctor may put you on nighttime oxygen or direct you to use a device such as a CPAP or BiPAP.
#5: Your Fingers or Lips Look Blue
Low oxygen levels can sometimes cause the fingers or lips to take on a blue tint, a condition known as cyanosis. This is usually more noticeable in more extreme cases, when someone’s oxygen levels are drastically low. It’s not that your hands aren’t getting any blood flow, rather that the blood is not full of the oxygen which gives it its red color. This is an indication that your oxygen levels have dipped dangerously low. If you notice your extremities turning blue, seek medical attention immediately, even if you are on oxygen already.
#6: Edema, or Swelling of the Feet or Ankles
Edema is fluid retention that tends to pool in feet or ankles. Swollen feet after a long walk in ill-fitting shoes is one thing, but if there’s no obvious cause for puffy feet or ankles, check in with your doctor.
People with COPD may experience swelling in the extremities as a result of having low blood oxygen levels over time. Your liver and kidneys are responsible for removing waste from the body. They need sufficient oxygen to do their job, which includes filtering toxins and fluids from the blood. When they aren’t getting enough oxygen, they can’t function properly, which may result in swelling of the extremities from fluid buildup. Gravity causes these fluids to mainly congregate in the lower extremities but can sometimes cause hands and arms to swell as well.
#7: Other Treatments Aren’t Helping
Most respiratory patients are placed on a corticosteroid inhaler. An inhaler can help reduce spasms in the airways and allow you to breathe more deeply, but it won’t improve oxygen levels the way oxygen therapy can. You’ll likely need a multi-pronged approach to treat your respiratory illness and its symptoms, so if you’re already using an inhaler and still feel short of breath or have trouble walking, adding oxygen therapy may be the next step
Don’t Wait!
Long term oxygen deprivation can cause serious and irreparable damage to cells and organs. Even after a few minutes of drastically low oxygen, your brain, liver, and other organs can suffer irreversible damage. If you are experiencing some or all of these symptoms, speak to your doctor right away.
The Most Serious Symptoms
- Severe Shortness of Breath
- Sudden Onset of Breathlessness
- Shortness of Breath when at Rest
- Being Startled Awake with Shortness of Breath or Choking Sensation
- Fluid Retention in Extremities
- Chronic Coughing or Wheezing
- Bluish Tint in Fingertips or Lips or Bright Redness
- Inability to Focus or Confusion
- Tightness in Chest
- Feeling Off Balance or Dizzy
- Excessive Sweating
If oxygen levels are low over an extended period of time it can cause neurological damage, organ failure, or even death. If your doctor has prescribed supplemental oxygen, don’t delay its use.
Oxygen Therapy

The effects of supplemental oxygen are immediate and have a positive impact on the heart, lungs, and brain. Your doctor will perform some or all of the diagnostic tests we’ve discussed if you are exhibiting symptoms of decreased blood oxygen. They will then decide if you are in need of supplemental oxygen therapy.
Supplemental oxygen therapy means that you will require a mechanism to provide you with more oxygen. This mechanism may be a pressurized tank with a regulator to release the oxygen via cannula to your nose. It can also be a portable device called a concentrator which produces medical oxygen by drawing in ambient air, filtering it through medical sieve, or zeolite, and delivering medical grade oxygen via cannula.
Using supplemental oxygen should reduce symptoms such a shortness of breath. It should also increase oxygen levels in your blood, reducing stress on your heart and lungs. If you’ve been suffering from sleep apnea or your oxygen has been dropping significantly during the night, it should also help you get deeper and more restful sleep. It will also leave you feeling more energetic and capable of carrying on with a normal and independent life.
Your Prescription
The doctor will decide if you need oxygen 24 hours a day or just in certain instances.
If your oxygen saturation goes down during the walk test but is fine other times, you may only have to use oxygen while exerting yourself. If you’re having trouble at night, your doctor may perform a sleep study and prescribe oxygen for nighttime use only.
Pulse Flow vs. Continuous Flow
Your doctor will either prescribe continuous or pulse flow oxygen. Many patients make the mistake of thinking that continuous means that you need oxygen continuously throughout the day. While you may need a constant flow of oxygen, continuous or pulse refers to the method of oxygen delivery. Pulse flow means that the concentrator can sense your inhalation and will deliver a bolus of oxygen only when you inhale.
If you require oxygen mostly during the day while active, you will likely need a pulse flow concentrator. If you require it 24/7 you may need a continuous flow of oxygen. If you have been prescribed a CPAP or BiPAP device, you must have a continuous flow concentrator.
Flow Rates
Continuous flow concentrator settings are measured in liters per minute. Setting 1 provides one liter of medical grade oxygen per minute, 2 provides 2 liters, and so on. It is estimated that 1 liter of oxygen will raise the patient’s oxygen saturation by about 3 – 4%. Everyone is different, of course, this is just a rough estimate. As of now the highest continuous oxygen concentrator provides 3 liters per minute of oxygen.
Pulse flow settings don’t correspond to liters. They are set by the manufacturer and may vary slightly from unit to unit. Your doctor may instruct you to use one level while sedentary and a higher level while exerting yourself. It will take careful monitoring during the first few months to arrive at your ideal dosage.
Nighttime Oxygen
As we said, if you must have a CPAP or BiPAP during the night you must have a continuous flow concentrator. If you don’t have a CPAP or BiPap, but still require nighttime oxygen, you will require a concentrator equipped with sleep mode, also known as intelligent delivery.
Intelligent delivery means that the concentrator can sense when the user inhales and will release a bolus or oxygen. Some release the bolus right at the beginning of inhalation and some released a measured dose throughout the entire inhalation cycle.
As your breathing gets shallower as you drift off to sleep, the machine will sense this and adjust it’s dose delivery accordingly to keep you properly titrated.
Once You Get Your Concentrator
Be sure to use it as directed. If you become short of breath or start having symptoms of hypoxia, don’t simply increase your oxygen settings. Just like any prescription medication, you should never adjust your dosage without consulting a physician. Doing so could make your condition worse or cause other physical issues.
Let us Know if We Can Help!
1st Class Medical is the largest distributor of portable oxygen concentrators in the world. This means we have access to all the latest models, have priority status for refurbished models, and have preferred pricing which we can pass on to you. You can visit us online or you can give us a call at 1-800-520-5726. We have factory trained technicians in our dedicated service center and we have an entire staff of respiratory specialists that are waiting to answer any questions you may have.
Please watch our O2 Classroom video about indications that you may need supplemental oxygen. Don’t forget to subscribe to our YouTube Channel where you can find more information about living with a respiratory disease.
































































Comments are closed